Last updated: February 17, 2026
Discovering blood on a mole can trigger immediate alarm, but is bleeding always bad? Not every bleeding mole signals cancer. Minor trauma from clothing, accidental scratching, or shaving can cause benign moles to bleed without indicating malignancy. However, spontaneous bleeding without injury, persistent oozing, or bleeding combined with other warning signs requires urgent professional evaluation because it may indicate melanoma ulceration or invasion.
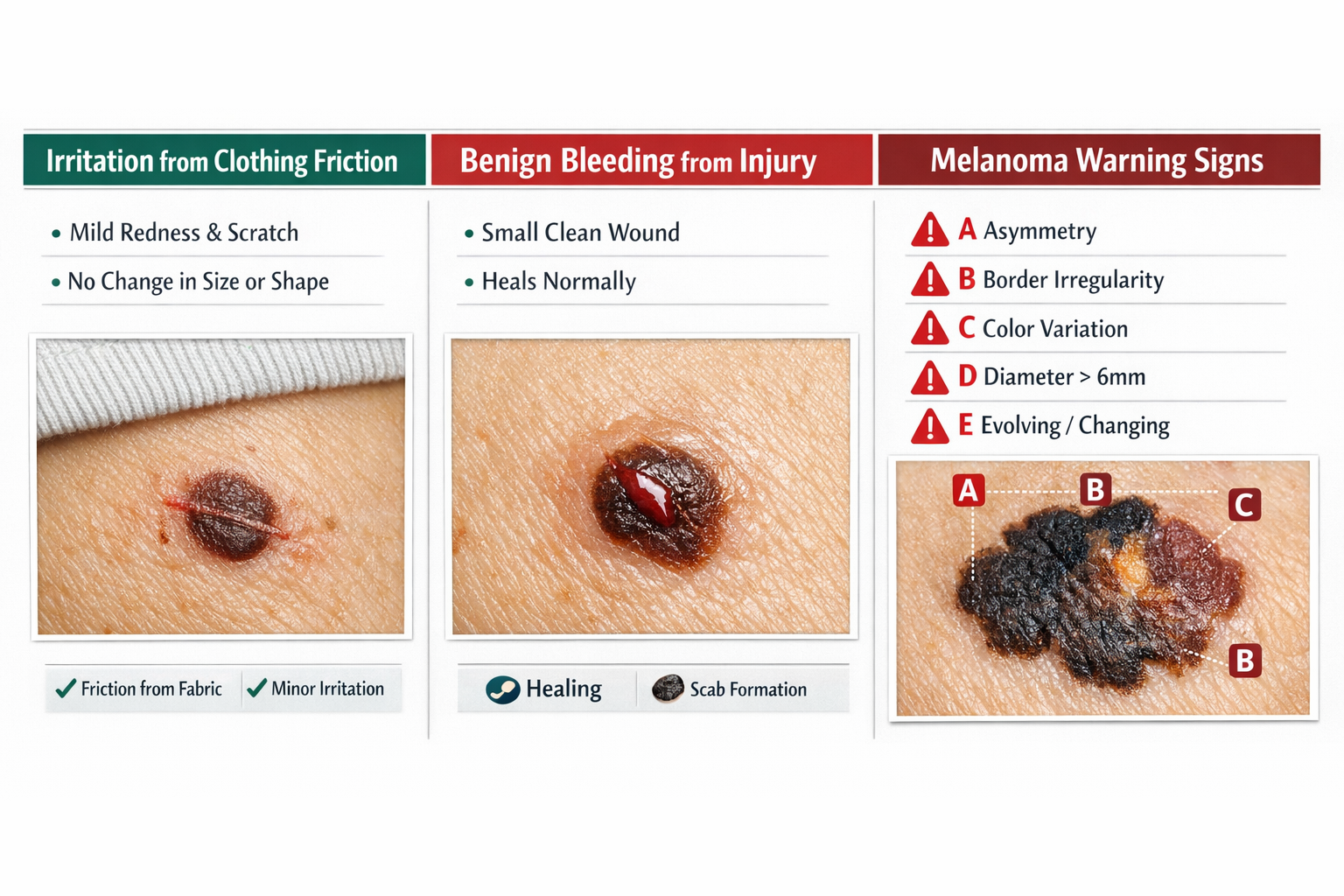
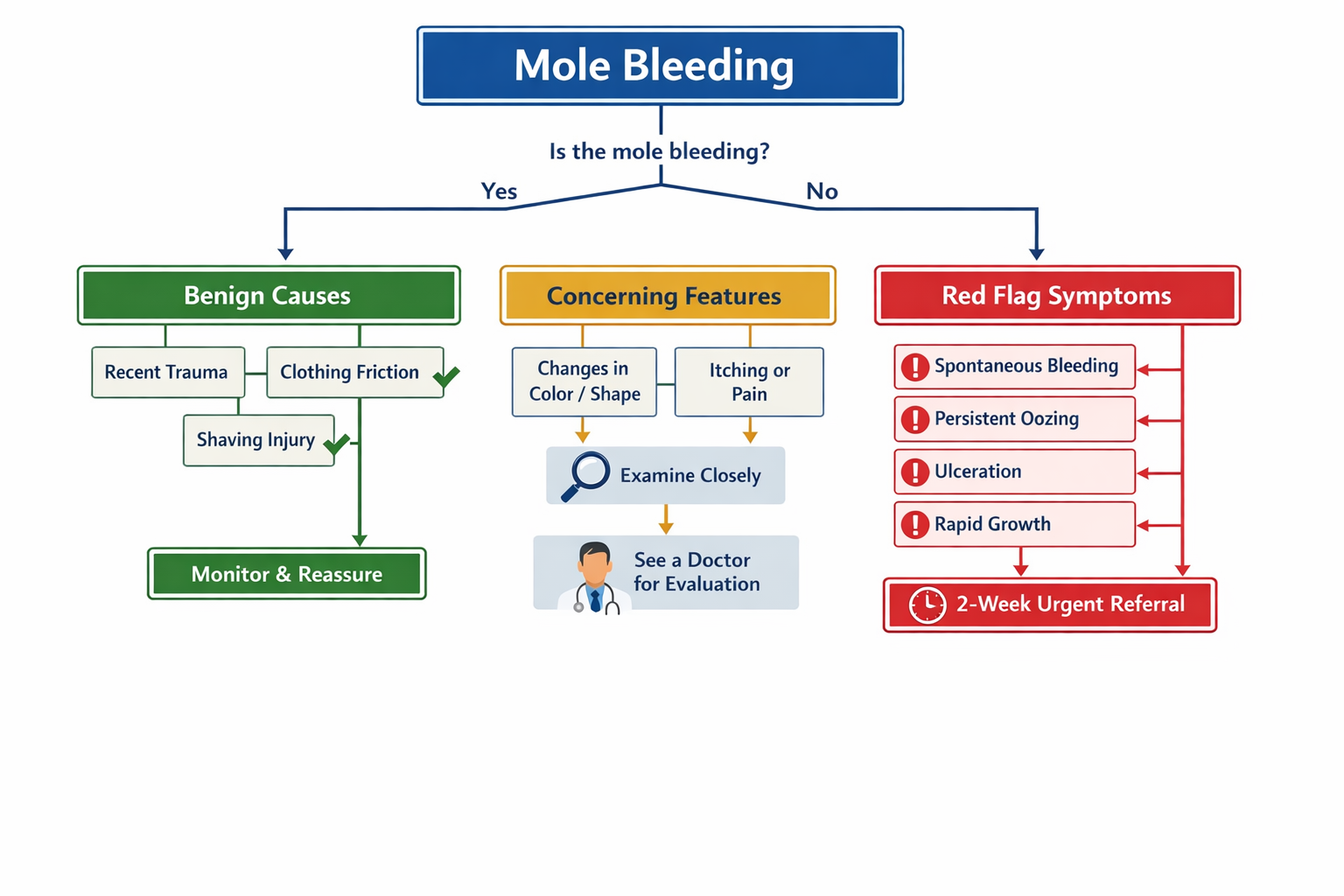
Bleeding from a mole after accidental trauma, shaving, or clothing friction is typically benign and stops with pressure. Spontaneous bleeding without injury, persistent oozing that doesn't heal, or bleeding combined with changes in size, shape, color, or texture signals possible melanoma and requires dermatology evaluation within 2 weeks. The critical distinction lies in whether the bleeding has an obvious external cause and resolves quickly versus recurring without explanation.
Normal moles can bleed for several innocent reasons that don't indicate cancer. Mechanical trauma represents the most common cause, including accidental scratching during sleep, aggressive towel drying, clothing friction from tight collars or bra straps, or direct injury during shaving or grooming. Raised moles positioned in high-friction areas like the neck, underarms, groin, or waistline are particularly vulnerable to repeated irritation.
Common benign bleeding triggers include:
Characteristics of benign bleeding:
Choose observation if: The bleeding episode has a clear traumatic cause, stops quickly with pressure, and the mole shows no other concerning changes. The surrounding skin heals normally within a few days, and the mole returns to its baseline appearance.
Common mistake: Assuming all bleeding requires immediate biopsy. Single traumatic bleeding episodes in stable moles with no other warning signs can be monitored with photographic documentation and follow-up assessment in 4-6 weeks.
For more information about distinguishing normal mole characteristics, see our guide on flat mole vs raised mole skin cancer risk.
The answer depends entirely on whether the bleeding has an identifiable external cause. Traumatic bleeding from accidental injury to a benign mole is not inherently concerning, provided the mole shows no other suspicious features and heals normally. Spontaneous bleeding without injury, however, indicates possible ulceration, a feature strongly associated with melanoma invasion and adverse prognosis.[1][2]
Traumatic bleeding characteristics:
Spontaneous bleeding red flags:
The British Association of Dermatologists emphasizes that any new persistent skin lesion that is bleeding should raise suspicion for melanoma and warrants specialist evaluation.[1] This guideline specifically addresses bleeding without obvious traumatic cause, distinguishing it from accidental injury to benign lesions.
Edge case: Some benign conditions like pyogenic granulomas (rapidly growing vascular bumps) can bleed easily with minor trauma but are not melanoma. These typically appear suddenly, grow rapidly over weeks, and have a distinctive bright red, raspberry-like appearance. Professional evaluation differentiates these benign vascular lesions from pigmented melanomas.
The ABCDE criteria provide a validated framework for melanoma detection, with bleeding representing a critical component of the "E" for evolution.[2][3] When bleeding occurs in combination with other ABCDE features, the likelihood of malignancy increases substantially, requiring urgent professional assessment.
A - Asymmetry: One half of the mole doesn't match the other half when divided through the center. Melanomas typically grow unevenly, creating lopsided or irregular shapes unlike the round or oval symmetry of benign moles.
B - Border irregularity: Edges appear jagged, scalloped, notched, or poorly defined rather than smooth and distinct. Melanoma borders often blur into surrounding skin or show irregular projections.
C - Color variation: Multiple colors within a single lesion, including shades of brown, black, red, white, or blue. Benign moles typically maintain uniform color throughout, while melanomas show uneven pigmentation patterns.
D - Diameter: Lesions larger than 6mm (pencil eraser size) warrant increased scrutiny, though melanomas can be smaller at early stages. Growing diameter over time is more concerning than static size.
E - Evolution: Any change in size, shape, color, elevation, or symptoms (bleeding, itching, crusting) over weeks to months. Stable moles that remain unchanged for years are typically benign, while evolving lesions require evaluation.[3]
Bleeding as an evolution indicator:
Bleeding without trauma signals possible ulceration, a feature indicating melanoma invasion through the epidermis. According to clinical guidelines, the combination of abnormal appearance and bleeding significantly increases the likelihood of malignant transformation.[1][2] Bleeding is specifically flagged as a possible indicator of melanoma ulceration, which affects staging and prognosis.[2]
The 7-point clinical checklist used by dermatologists assigns weighted scores:
Major features (2 points each):
Minor features (1 point each):
A total score of 3 or more points indicates higher suspicion requiring professional referral.[2] This expanded framework provides diagnostic depth beyond basic ABCDE self-examination.
For comprehensive evaluation criteria, review our suspicious mole checklist.
Changes in mole sensation or surface characteristics often accompany bleeding in melanomas. Itching, bleeding, and crusting are warning signs of melanoma and should be evaluated promptly by a dermatologist.[3][6] These symptoms indicate inflammatory changes, nerve involvement, or possible ulceration that extends beyond simple mechanical irritation.[2]
Concerning symptom combinations:
Differentiate from benign conditions:
Seborrheic keratoses (benign age-related growths) can become irritated, itchy, and develop surface crusting but typically appear waxy, stuck-on, and clearly distinct from surrounding skin. Dermatitis or eczema causes itching across broader areas rather than isolated to a single lesion. Contact irritation from new skincare products affects multiple sites rather than one specific mole.
When to seek evaluation:
Any mole showing persistent symptoms lasting more than 2-3 weeks despite avoiding irritation warrants professional assessment. Symptoms that progressively worsen, occur spontaneously without external triggers, or combine with visual changes (size, color, shape) require urgent dermatology referral within 2 weeks.[1]
Common mistake: Attributing persistent itching or crusting to dry skin or minor irritation when the symptoms are localized to a changing pigmented lesion. Benign dry skin affects broad areas and responds to moisturization, while melanoma-associated symptoms persist despite appropriate skincare.
The "ugly duckling" sign provides comparative assessment by identifying lesions that appear different from the patient's other moles.[1][2] Humans typically develop moles with similar characteristics based on genetic factors and sun exposure patterns. A mole that stands out as distinctly different in color, size, shape, or behavior warrants professional evaluation, even without meeting all ABCDE criteria.
How to apply the ugly duckling concept:
Examine all visible moles on the body and identify overall patterns. Most people have moles that resemble each other in general appearance—similar colors (light brown, medium brown, or dark brown), similar sizes (mostly small or mostly medium), and similar shapes (mostly flat or mostly slightly raised).
Ugly duckling indicators:
This comparative approach proves particularly valuable for detecting nodular melanoma, an aggressive subtype that may not follow traditional ABCDE rules. Nodular melanomas can be symmetrical, uniformly colored, and smaller than 6mm but still dangerous because they grow vertically (deeper) rather than horizontally (wider).[2]
The EFG rule for nodular melanoma:
Nodular melanomas require supplementary vigilance because they may be missed by standard ABCDE criteria and can present as a raised bump without dark pigmentation.[2] The ugly duckling sign helps identify these atypical presentations.
Edge case: Patients with atypical mole syndrome (dysplastic nevus syndrome) may have many unusual-appearing moles that differ from each other. These individuals require professional mole mapping, baseline photography, and regular dermatology monitoring rather than relying on self-examination alone.
Learn more about unusual presentations in our article on amelanotic melanoma.
Professional evaluation of bleeding moles follows a systematic protocol combining clinical examination, dermoscopy, and appropriate biopsy when indicated. Lesions suspicious for melanoma should NOT be removed in primary care settings.[1] The British Association of Dermatologists emphasizes that urgent referral to dermatology or a skin cancer multidisciplinary team should occur within 2 weeks, with complete excisional biopsy as the diagnostic standard.[1]
Clinical examination components:
Visual inspection under good lighting assesses asymmetry, border characteristics, color variation, and diameter. The dermatologist documents lesion location, size measurements, and photographic records for comparison at follow-up visits.
Dermoscopy (also called dermatoscopy) uses a specialized magnifying device with polarized light to examine subsurface structures invisible to the naked eye. Dermoscopic patterns help differentiate benign lesions from melanomas with significantly improved diagnostic accuracy compared to visual examination alone.
Patient history includes:
Biopsy decision-making:
Complete excisional biopsy with 2mm clinical margin is required for accurate diagnosis when melanoma is suspected.[1] This removes the entire lesion with a narrow margin of normal-appearing skin, allowing pathologists to examine the full depth and architecture of the growth.
Shave biopsies and punch biopsies are absolutely contraindicated for suspected melanomas because they lead to sampling error, incorrect diagnosis, and make accurate pathological staging impossible.[1] Partial sampling may miss the most atypical area or fail to determine the true depth of invasion, both critical for treatment planning.
Biopsy is recommended when:
Observation may be appropriate when:
For those concerned about the biopsy process, read our guide addressing does mole removal hurt.
When melanoma is diagnosed, the presence of bleeding or ulceration indicates possible invasion and higher stage disease, affecting both treatment planning and prognosis.[1] Ulceration represents a break in the epidermis overlying the melanoma, often manifesting clinically as bleeding, oozing, or persistent crusting.
Staging implications:
Melanoma staging uses the TNM system (Tumor, Nodes, Metastasis) with ulceration as a critical T-stage modifier. For melanomas of the same thickness, the presence of ulceration automatically upstages the lesion because it indicates more aggressive biology.
Breslow thickness categories with ulceration impact:
ThicknessWithout UlcerationWith Ulceration≤1.0 mmT1a (excellent prognosis)T1b (good prognosis, may need sentinel node biopsy)1.01-2.0 mmT2a (good prognosis)T2b (moderate prognosis, sentinel node biopsy recommended)2.01-4.0 mmT3a (moderate prognosis)T3b (guarded prognosis, sentinel node biopsy recommended)>4.0 mmT4a (guarded prognosis)T4b (poor prognosis, aggressive workup needed)
Sentinel lymph node biopsy consideration:
Ulcerated melanomas, even when thin (<1mm), may warrant sentinel lymph node biopsy to detect microscopic spread.[1] This staging procedure identifies early lymph node involvement that affects treatment decisions and follow-up intensity.
Prognostic significance:
Ulceration indicates more aggressive melanoma behavior with higher risk of recurrence and metastasis compared to non-ulcerated melanomas of similar thickness. The biological mechanisms include increased angiogenesis (blood vessel formation), inflammatory response, and tumor invasion through the basement membrane.
Treatment modifications:
Ulcerated melanomas typically require:
Understanding these staging implications underscores why spontaneous bleeding from a pigmented lesion requires urgent evaluation rather than watchful waiting. Early detection before ulceration develops offers significantly better outcomes.
For information about follow-up protocols after melanoma diagnosis, consult resources on melanoma staging and follow-up.
Certain populations face elevated melanoma risk and require heightened surveillance, with any bleeding mole warranting particularly urgent evaluation. High-risk patients benefit from monthly self-examination and professional monitoring with baseline photography and dermoscopy.[1]
High-risk factors requiring enhanced vigilance:
Age and skin type:
Mole characteristics:
Personal medical history:
Family history:
Enhanced monitoring protocols for high-risk patients:
Monthly self-examination using the ABCDE criteria, ugly duckling sign, and photographic documentation of concerning lesions. Professional full-body skin examination every 3-6 months with dermoscopy and baseline mole mapping. Consider advanced imaging like sequential digital dermoscopy for tracking subtle changes over time.
Choose professional mole mapping if: You have more than 50 moles, a personal or family history of melanoma, or atypical mole syndrome. Baseline photography allows objective comparison over time, detecting subtle changes that might be missed by memory alone.
For those seeking professional evaluation, explore mole mapping clinics in Toronto or find a skin cancer clinic near you.
When a mole bleeds, immediate response depends on whether the bleeding has an obvious traumatic cause and whether other warning signs are present. Appropriate initial management combined with timely professional evaluation ensures both practical wound care and cancer detection when needed.
Immediate steps for any bleeding mole:
When to seek same-day or next-day evaluation:
When to schedule urgent dermatology evaluation (within 2 weeks):
When observation with follow-up may be appropriate:
Common mistake: Delaying evaluation for weeks or months while "watching" a concerning mole that shows multiple warning signs. The 2-week urgent referral guideline exists because early melanoma detection dramatically improves outcomes, with 5-year survival rates exceeding 99% for localized disease versus 30% for metastatic disease.
Edge case: Patients on anticoagulation therapy (blood thinners like warfarin, apixaban, or aspirin) may experience prolonged bleeding from minor trauma. While this explains extended bleeding duration, it doesn't eliminate the need to evaluate the mole itself for concerning features. Focus assessment on whether the mole shows warning signs beyond the bleeding episode.
Find a qualified provider through our directory of best mole removal clinics.
Several benign conditions can present with bleeding or concerning appearance, requiring professional differentiation from melanoma. Understanding these mimics helps contextualize symptoms while emphasizing that definitive diagnosis requires expert evaluation rather than self-diagnosis.
Pyogenic granuloma (lobular capillary hemangioma):
A rapidly growing vascular lesion that bleeds easily with minor trauma. Typically appears as a bright red, raspberry-like bump that develops over weeks, often at sites of previous injury. Most common in children and young adults, particularly on fingers, lips, and gums. Benign but requires removal due to persistent bleeding tendency.
Seborrheic keratosis:
Benign age-related growths with waxy, stuck-on appearance that can become irritated, itchy, and bleed when traumatized. Usually multiple lesions with tan, brown, or black color. Surface may appear scaly or warty. Common after age 40 and increases with age. Distinguished from melanoma by characteristic appearance on dermoscopy.
Dermatofibroma:
Firm, benign fibrous nodules that may appear brown or pink and can bleed if scratched or shaved. Typically feel like a hard button under the skin and dimple inward when squeezed from the sides. Common on legs, especially in women. Usually asymptomatic but may be tender.
Learn to differentiate these lesions in our guide on dermatofibroma vs skin cancer.
Traumatized nevus (benign mole with injury):
A normal mole that has been accidentally cut, scraped, or irritated may develop bleeding, crusting, and inflammation that resolves with healing. The key distinction is clear traumatic history and return to baseline appearance after complete healing within 2-3 weeks.
Hemangioma:
Benign vascular birthmarks or acquired vascular lesions that can bleed with trauma. Bright red or purple color, blanch partially with pressure, and have characteristic dermoscopic patterns. May be flat or raised depending on type.
Angiokeratoma:
Small vascular lesions with overlying hyperkeratosis (thickened skin) that appear as dark red to black papules. Can bleed with trauma but are benign. Common on scrotum, vulva, and extremities.
Why professional evaluation is essential:
While these benign conditions exist, patients cannot reliably self-diagnose. Melanomas can mimic benign lesions, and benign lesions can have atypical features. Dermoscopy and, when appropriate, biopsy provide definitive diagnosis. The risk of delaying melanoma diagnosis far outweighs the inconvenience of evaluating a benign lesion.
Diagnostic approach:
Dermatologists use dermoscopy to identify specific patterns characteristic of benign versus malignant lesions. When dermoscopic features are equivocal or concerning, excisional biopsy provides histopathological diagnosis. The pathologist examines tissue architecture, cell morphology, and growth patterns to definitively classify the lesion.
Understanding common errors in mole assessment helps patients and primary care providers recognize when specialist referral is necessary rather than attempting prolonged observation or inappropriate treatment.
Mistake 1: Assuming traumatic bleeding eliminates cancer concern
While trauma explains the bleeding episode itself, it doesn't confirm the underlying lesion is benign. Melanomas can bleed with minor trauma that wouldn't affect normal skin. The critical assessment is whether the mole shows other warning signs beyond the bleeding incident.
Correction: Evaluate the mole using ABCDE criteria regardless of identified trauma. If other concerning features exist, refer for dermatology evaluation even when bleeding has an obvious cause.
Mistake 2: Prolonged observation of changing lesions
Waiting months to "see what happens" with a mole showing progressive changes delays diagnosis during the critical window when melanoma is most treatable. The 2-week urgent referral guideline exists because early detection dramatically improves outcomes.
Correction: Any mole showing progressive change over weeks to months warrants evaluation, not extended observation. Document with photography and refer within 2 weeks if concerning features are present.
Mistake 3: Performing shave biopsy on suspected melanoma
Shave biopsies remove only the superficial portion of a lesion and are absolutely contraindicated for suspected melanomas.[1] This technique prevents accurate depth measurement (Breslow thickness), the most important prognostic factor, and may lead to incorrect staging and inadequate treatment.
Correction: Suspected melanomas require complete excisional biopsy with narrow margins, removing the entire lesion for full-thickness pathological examination.[1] Refer to dermatology or surgical specialists trained in melanoma management.
Mistake 4: Reassuring patients based solely on lesion size
While diameter >6mm is part of ABCDE criteria, melanomas can be smaller, especially at early stages. Nodular melanomas may be small but deeply invasive. Size is one criterion among many, not a standalone reassurance.
Correction: Evaluate all ABCDE criteria plus evolution, ugly duckling sign, and patient risk factors. Small changing lesions in high-risk patients warrant the same urgency as larger lesions.
Mistake 5: Attributing all symptoms to benign causes
Persistent itching attributed to dry skin, crusting blamed on eczema, or bleeding explained by clothing friction may delay melanoma diagnosis when symptoms are actually tumor-related.
Correction: Symptoms localized to a single changing pigmented lesion require evaluation for melanoma, even when alternative explanations seem plausible. Benign conditions typically affect broader areas and respond to appropriate treatment.
Mistake 6: Ignoring amelanotic (non-pigmented) melanomas
Melanomas lacking typical brown or black pigmentation account for 0.4-27.5% of cases and may present as pink, red, or flesh-colored lesions.[1] These atypical presentations are easily dismissed as benign bumps or irritation.
Correction: Evaluate all new or changing skin lesions, regardless of color. Amelanotic melanomas often present with bleeding, rapid growth, or ulceration as the primary warning signs when pigmentation is absent.
Read more about this challenging diagnosis in our article on amelanotic melanoma.
Is bleeding from a mole always a sign of cancer?
No, bleeding from a mole is not always cancer. Accidental trauma from shaving, scratching, or clothing friction commonly causes benign moles to bleed. However, spontaneous bleeding without injury or persistent bleeding that recurs is a melanoma warning sign requiring urgent dermatology evaluation within 2 weeks.[1][2]
How can I tell if mole bleeding is serious?
Serious bleeding has no identifiable traumatic cause, recurs without additional injury, doesn't heal within 2 weeks, or occurs with other warning signs like asymmetry, irregular borders, color changes, or rapid growth. Single episodes after clear trauma that stop with pressure and heal normally are typically less concerning.
Should I see a doctor immediately if my mole bleeds?
See a doctor within 2 weeks if bleeding is spontaneous, recurrent, or accompanied by other ABCDE warning signs.[1] Seek same-day evaluation if bleeding doesn't stop after 15 minutes of pressure, involves significant blood loss, or shows signs of infection. Single traumatic bleeding with clear cause and no other concerns can be monitored with follow-up in 4-6 weeks.
Can a normal mole bleed if I scratch it?
Yes, normal benign moles can bleed when scratched, scraped, or injured. The bleeding typically stops within 5-10 minutes with gentle pressure and heals normally within a few days. The key is whether the mole shows other concerning features beyond the traumatic bleeding episode.
What does melanoma bleeding look like?
Melanoma bleeding may appear as spontaneous oozing without injury, persistent seepage that creates recurring crusts, or surface breakdown (ulceration) with visible raw areas. The bleeding often doesn't fully heal between episodes and may be accompanied by changes in the lesion's size, shape, or color.
How long should I wait to see if a bleeding mole heals?
If bleeding occurred from clear trauma and the mole shows no other warning signs, allow 2 weeks for complete healing while monitoring for changes. If bleeding is spontaneous, recurs, or the mole shows ABCDE warning signs, schedule dermatology evaluation within 2 weeks rather than waiting.[1]
Can shaving cause a mole to bleed and turn cancerous?
Shaving can cause a benign mole to bleed through mechanical trauma, but the injury itself doesn't cause cancer. However, if a mole bleeds very easily from minimal trauma or doesn't heal properly, it may indicate an underlying problem requiring evaluation. The trauma reveals the issue rather than creating it.
For concerns about mole removal procedures, read our guide on whether removing a mole causes cancer.
What should I do if my mole keeps bleeding?
Persistent or recurrent bleeding without repeated trauma requires dermatology evaluation within 2 weeks.[1] Document the bleeding episodes with dates and photographs, avoid further irritation, and do not attempt home treatment. Recurrent bleeding is a red flag for possible melanoma ulceration.
Are bleeding moles more common in certain body areas?
Moles in high-friction areas (neck, underarms, groin, waistline, bra line) experience more traumatic bleeding from clothing and movement. However, spontaneous bleeding can occur anywhere and is concerning regardless of location. Scalp, back, and leg melanomas are particularly dangerous because they may go unnoticed longer.
Can a mole bleed internally without visible blood?
Moles don't typically "bleed internally" in the way deeper tissues can. However, melanomas may develop internal vascular changes visible only on dermoscopy or pathology. Any color changes toward red, blue, or white within a mole may indicate vascular changes and warrant evaluation.
Is it normal for a mole to bleed after exercise?
Benign moles don't normally bleed from exercise alone unless friction from clothing or equipment causes mechanical trauma. If a mole bleeds repeatedly during exercise without obvious rubbing or injury, evaluation is warranted to rule out a friable (easily bleeding) lesion.
How do I stop a mole from bleeding at home?
Apply gentle, continuous pressure with clean gauze or cloth for 5-10 minutes without repeatedly checking. Once bleeding stops, clean gently with mild soap and water, apply antibiotic ointment, and cover with a bandage. If bleeding doesn't stop after 15 minutes of pressure, seek medical evaluation.
Is bleeding always bad? The answer requires context, clinical judgment, and appropriate urgency. Bleeding from a mole after accidental injury typically represents benign trauma to normal tissue, resolving quickly with basic wound care. However, spontaneous bleeding without identifiable cause, persistent oozing that doesn't heal, or bleeding combined with other ABCDE warning signs demands immediate professional evaluation because it may indicate melanoma ulceration and invasion.
The critical distinction lies not in the bleeding itself but in the complete clinical picture: What caused the bleeding? Does it recur? What does the mole look like? Is it changing? Does it stand out from other moles? What are the patient's risk factors?
Your action plan:
For a single bleeding episode with clear traumatic cause:
For spontaneous or recurrent bleeding:
For high-risk patients:
The stakes are too high for guesswork. Melanoma detected at early stages offers excellent prognosis with simple surgical treatment, while delayed diagnosis allows progression to advanced disease with dramatically worse outcomes. When doubt exists, professional evaluation provides definitive answers and peace of mind.
Don't let fear of "overreacting" delay potentially life-saving diagnosis. Dermatologists would rather evaluate ten benign lesions than miss one early melanoma. Your vigilance, combined with appropriate professional assessment, creates the best opportunity for early detection and successful treatment.
If you're concerned about a bleeding mole or any changing skin lesion, schedule an evaluation at a qualified skin cancer clinic or mole removal center in your area. Your skin health deserves expert attention, and early action makes all the difference.
[1] What Is The Diagnosis And Icd 10 International Classification Of - https://www.droracle.ai/articles/758621/what-is-the-diagnosis-and-icd-10-international-classification-of
[2] Suspicious Mole Checklist The Complete 2026 Guide - https://www.theminorsurgerycenter.com/blog/suspicious-mole-checklist-the-complete-2026-guide
[3] Melanoma Detection Abcde Guide - https://www.psdermgroup.com/melanoma-detection-abcde-guide
[6] Mole Patrol When Changes Signal Its Time To See A Dermatologist - https://doralhw.org/mole-patrol-when-changes-signal-its-time-to-see-a-dermatologist/