Quick Answer: Doctors check a mole for cancer by reviewing its history, examining its size, shape, colour, border, surface texture, and symptoms, and looking for ABCDE warning signs. If a mole looks suspicious, a biopsy or excision is recommended. The removed tissue is sent to a pathology lab, which confirms whether the mole is benign, atypical, or cancerous.
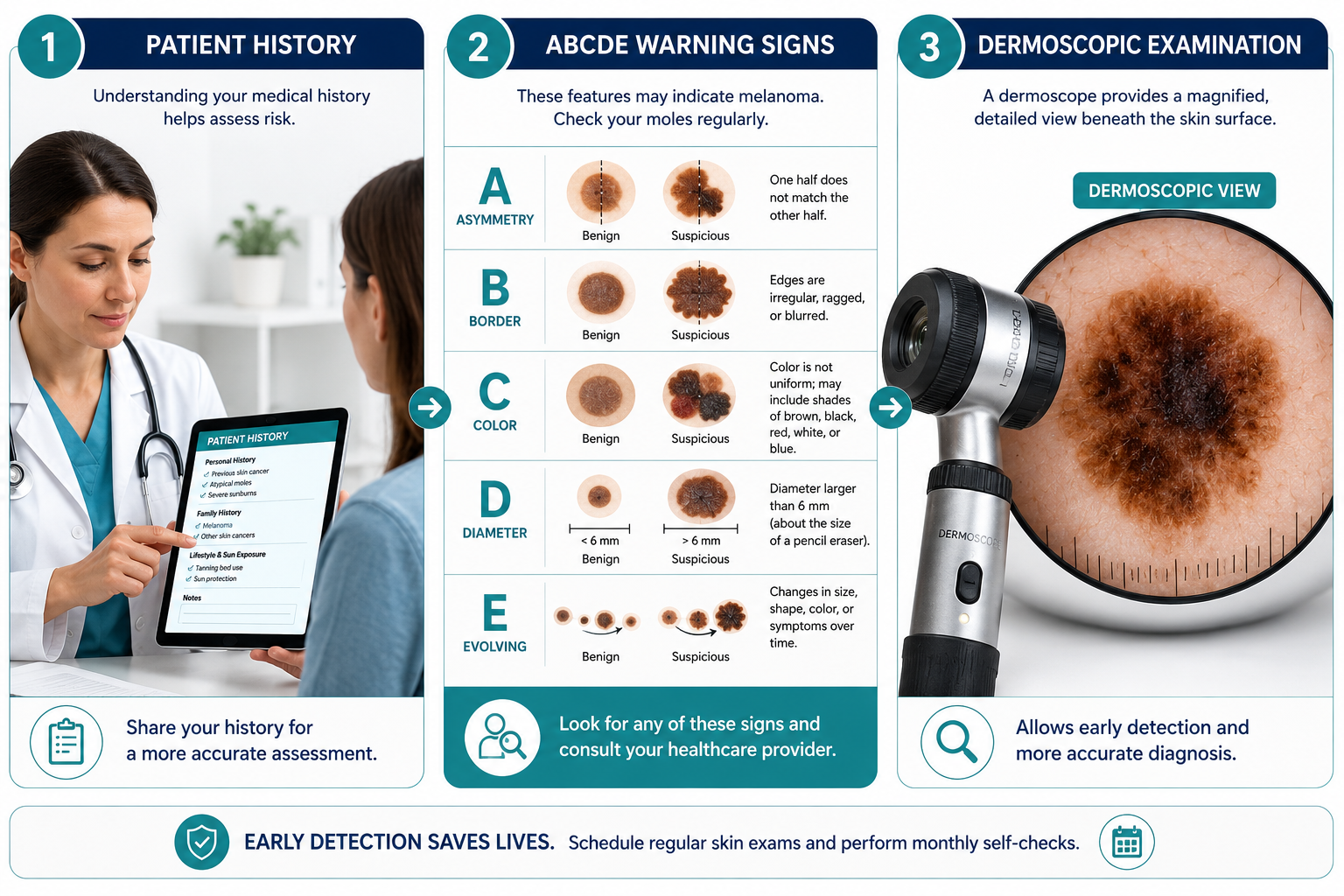
A mole check follows a clear, structured process. The doctor reviews the mole's history, examines it visually (with or without a dermoscope), applies the ABCDE criteria, and then decides whether to monitor, photograph, or biopsy the lesion.
Most appointments take 15 to 30 minutes for a focused mole check, or longer for a full-body skin examination. No needles or cutting are involved unless a biopsy is needed. The exam itself is painless.
Here is what the process looks like from start to finish:
Before looking at the mole, the doctor asks a series of targeted questions. The answers help determine how urgently the mole needs attention.
Common questions include:
Bringing older photos is genuinely useful. A mole that looks slightly irregular but has been stable for a decade is very different from one that doubled in size over three months. Change over time is one of the most important signals a doctor looks for [9].
Patients with a history of previous skin cancers, dysplastic nevi, or a first-degree relative with melanoma are considered higher risk and may be referred for more thorough screening. For a deeper look at how skin cancer screening works, see this complete guide to skin cancer screening in Toronto.
The doctor examines the mole under good lighting, often using a handheld dermoscope (a magnified, polarized light device) to see structures beneath the skin surface that are invisible to the naked eye.
What the doctor assesses:
FeatureWhat They Look ForShapeRound and symmetrical vs. irregular or asymmetricalBorderSmooth and well-defined vs. ragged, notched, or blurredColourSingle uniform tone vs. multiple shades (brown, black, red, white, blue)SizeDiameter relative to a pencil eraser (~6 mm)SurfaceFlat, raised, smooth, scaly, ulcerated, or crustedSurrounding skinRedness, satellite lesions, swelling
Dermoscopy improves melanoma detection accuracy by approximately 49% compared to the naked eye alone, and experienced dermatologists achieve melanoma detection rates roughly 13 times higher than general practitioners using dermoscopy [4][10]. This is why seeing a physician with specific skin cancer training matters.
The ABCDE rule is the standard clinical framework for evaluating suspicious moles. It was developed to give both clinicians and patients a consistent checklist [5][9].
ABCDE Breakdown:
Important caveat: The naked-eye ABCDE assessment has a sensitivity of approximately 71% for melanoma detection, while dermoscopy raises that to around 90% [10]. A mole can have one or two ABCDE features and still be benign, or it can look unremarkable and still require biopsy based on the patient's overall risk profile.
"The ABCDE rule is a starting point, not a final answer. Dermoscopy and pathology complete the picture."
After the history and examination, the doctor makes one of three recommendations:
Option A: Monitor (watch and wait)
The mole shows no significant warning signs and the patient has no high-risk history. The doctor may photograph the mole and schedule a follow-up in 3 to 12 months to check for change.
Option B: Biopsy
The mole has suspicious features but the diagnosis is unclear. A tissue sample is taken and sent to pathology. This is the most common next step for a mole that raises concern.
Option C: Excision (full removal)
The mole looks highly suspicious, or the patient wants it removed regardless. The entire mole is removed with a margin of surrounding normal skin and sent to pathology simultaneously.
Choose monitoring if: The mole is stable, symmetrical, single-coloured, and the patient has no risk factors.
Choose biopsy if: One or more ABCDE features are present, the mole has changed recently, or the patient has a history of atypical moles or melanoma.
Choose excision if: The mole is highly suspicious, large, or the patient prefers removal for peace of mind.
For patients in the Greater Toronto Area, the Minor Surgery Center's mole removal and skin cancer services offer both biopsy and excision options with on-site pathology submission.
If a biopsy or excision is performed, the removed tissue is placed in a preservative solution and sent to a certified pathology laboratory. A pathologist examines the tissue under a microscope and issues a formal report.
Pathology classifies the mole as one of the following:
To understand what your pathology report means after mole removal, see this guide to interpreting your pathology report.
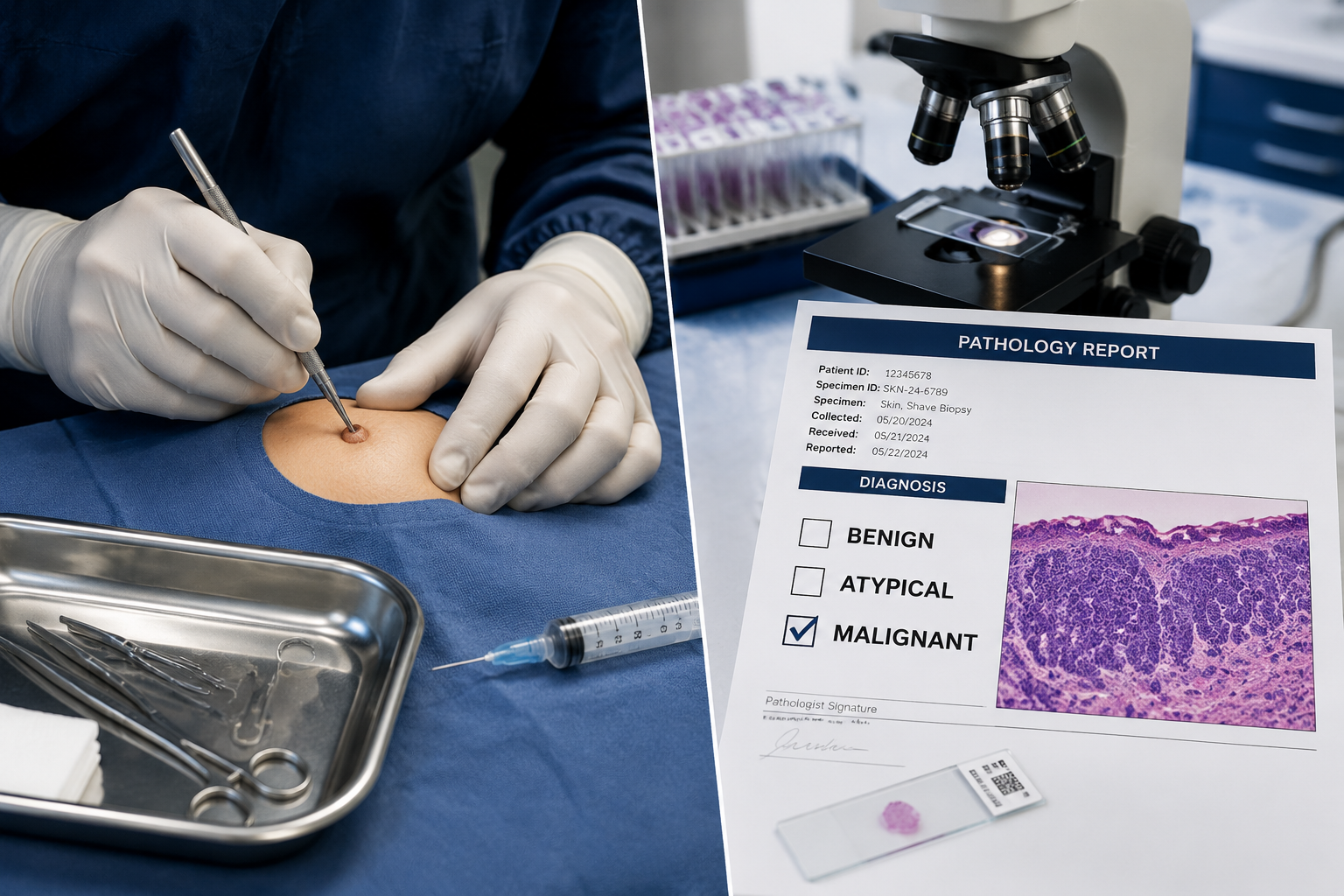
A mole biopsy is a minor outpatient procedure. The examination itself does not hurt at all. If a biopsy is needed, local anesthetic is injected into the skin around the mole before any tissue is removed. Most patients describe the anesthetic injection as a brief sting or pinch lasting a few seconds, after which the area is completely numb.
There are three main biopsy techniques. The choice depends on the mole's size, depth, location, and how suspicious it looks.
1. Shave Biopsy
A thin blade shaves the mole flush with the surrounding skin. Used for raised moles that appear superficial. Quick, leaves a shallow wound that heals without stitches in most cases.
2. Punch Biopsy
A circular cutting tool removes a small, full-thickness core of skin (typically 2 to 6 mm in diameter). Used when the doctor needs to assess the full depth of the lesion. May require one or two stitches.
3. Excisional Biopsy
The entire mole is cut out with a scalpel along with a small margin of normal surrounding skin. This is both a diagnostic and potentially curative procedure. Stitches are required. Most appropriate for highly suspicious moles.
After the procedure:
For patients wondering about stitches specifically, this article on whether mole removal requires stitches covers what to expect based on the technique used.
Visual assessment can identify suspicious features, but it cannot confirm cancer. Only pathology can do that.
Even the most experienced dermatologist using dermoscopy cannot guarantee a diagnosis from visual inspection alone. Dermoscopy achieves approximately 90% sensitivity for melanoma detection, which is significantly better than the naked eye, but it still leaves room for uncertainty [10]. A mole that looks completely normal can occasionally harbour early malignant cells, and a mole with multiple ABCDE features can turn out to be benign.
What visual assessment can do:
What visual assessment cannot do:
This is why the standard of care always involves pathology for any mole that raises clinical concern. For context on the different types of skin cancer that pathology may identify, see this guide to the 4 main types of skin cancer.
AI-assisted mole assessment is advancing rapidly. A January 2026 review in PMC found that AI systems match clinician accuracy for melanoma detection, with some models achieving 80.9% sensitivity and 75.6% specificity, comparable to dermatologists' 78.6% sensitivity and 75.2% specificity [10].
A major Swedish study published in April 2026 showed that AI models using routine health data (age, diagnoses, medications, demographics) could identify high-risk melanoma groups with up to 33% five-year risk, achieving 73% accuracy versus 64% for age and sex alone [8]. Researchers from the University of Gothenburg analyzed data from 6 million Swedes, finding that 0.64% developed melanoma over five years, and AI could efficiently target the highest-risk subset for proactive screening [8].
In April 2026, a company called SquareMind raised $18 million for a robotic whole-body scanning system designed to map every mole and track changes automatically, aiming to make population-level skin cancer screening more systematic [6].
These tools are promising, but as of 2026, none have replaced the clinical examination and pathology biopsy as the diagnostic standard. AI currently functions as a triage and risk-stratification tool rather than a standalone diagnostic.
Pathology provides the definitive answer about a mole's nature. The report describes the cellular characteristics of the removed tissue and classifies the lesion precisely.
Key information in a pathology report:
What happens next depends on the result:
ResultTypical Next StepBenign nevusNo further treatment; routine skin checksMild dysplastic nevus with clear marginsMonitor; no re-excision needed in most casesModerate/severe dysplastic nevusRe-excision to ensure clear marginsMelanoma in situWide local excision (usually 5 mm margins)Invasive melanomaWide excision + sentinel lymph node biopsy depending on depthBasal or squamous cell carcinomaExcision with appropriate margins; rarely more
For a full explanation of how to read your results, the pathology report guide after mole removal walks through each section of the report in plain language.
Book a mole check promptly if any of the following apply. Do not wait for an annual physical if a mole is changing rapidly.
Book urgently (within 1 to 2 weeks) if:
Book for a routine check if:
Who is at higher risk and should be screened regularly:
Dr. Darrell Rigel, presenting at Winter Clinical 2026, projected more than 112,000 invasive melanoma diagnoses in the United States for 2026, underscoring that melanoma rates continue to rise and early screening remains the most effective intervention available [7].

For patients in Toronto and the surrounding Greater Toronto Area, several clinic types offer mole checks, biopsy, and excision services.
Options include:
The Minor Surgery Center operates across multiple GTA locations and offers same-day mole assessment, biopsy, and excision with pathology submission. Locations include:
For a broader overview of the best skin cancer clinics in the GTA, including what to look for when choosing a provider, that resource covers credentials, wait times, and what questions to ask.
How do doctors check a mole for cancer?
Doctors review the mole's history (when it appeared, whether it changed, symptoms), examine its size, shape, colour, border, and surface using the ABCDE criteria, often with a dermoscope. If it looks suspicious, they recommend a biopsy or excision and send the tissue to pathology for a definitive diagnosis [5][9].
Can a doctor tell if a mole is cancerous just by looking at it?
No. Visual assessment and dermoscopy can identify suspicious features with high accuracy, but only pathology (microscopic analysis of removed tissue) can confirm whether a mole is cancerous. Even experienced dermatologists using dermoscopy achieve around 90% sensitivity, not 100% [10].
What happens during a mole check appointment?
The doctor asks about the mole's history, examines it visually (with or without a dermoscope), assesses ABCDE features, and recommends monitoring, biopsy, or removal. The exam itself is painless and takes 15 to 30 minutes for a focused check [4].
Does a mole check hurt?
The visual examination does not hurt at all. If a biopsy is needed, a local anesthetic injection causes a brief sting lasting a few seconds. After that, the area is numb and the procedure is painless.
When does a mole need a biopsy?
A biopsy is recommended when a mole shows one or more ABCDE warning signs, has changed recently, bleeds or itches persistently, looks unlike the patient's other moles, or when the doctor cannot confidently classify it as benign on visual inspection alone [9].
How is a mole biopsy done?
The skin is cleaned and numbed with local anesthetic. The doctor then removes the mole using a shave technique (thin blade), punch technique (circular cutter), or excisional technique (scalpel with margins). The tissue is sent to a pathology lab. The procedure takes 10 to 20 minutes in most cases.
Is a mole biopsy painful?
The biopsy itself is not painful because local anesthetic is used. The injection of anesthetic may cause a brief stinging sensation. After the procedure, mild soreness for 1 to 3 days is normal and managed with over-the-counter pain relief.
How long do mole biopsy results take?
Pathology results typically return within 1 to 2 weeks. Urgent cases flagged by the surgeon may be processed faster. The clinic will contact the patient when results are available and schedule a follow-up if needed.
What does pathology show after mole removal?
The pathology report classifies the mole as benign, atypical (dysplastic, graded mild/moderate/severe), or malignant (cancerous). For melanoma, it also reports Breslow thickness, margins, mitotic rate, and ulceration, which determine staging and next treatment steps.
Can a mole be removed and tested at the same time?
Yes. Excisional biopsy removes the entire mole with a margin of normal skin in a single procedure. The removed tissue is then sent to pathology. This approach is both diagnostic and potentially curative if the mole turns out to be an early-stage cancer with clear margins.
How often should I get a mole check?
Annual full-body skin exams are recommended for adults with risk factors (fair skin, family history, many moles, prior skin cancer). People without risk factors should still have moles checked if they notice any changes. High-risk patients may need checks every 3 to 6 months [1].
What is the "ugly duckling" sign?
The ugly duckling sign is a clinical concept where a mole that looks noticeably different from all of a patient's other moles is flagged as suspicious, even if it does not meet classic ABCDE criteria. It is a useful supplement to the ABCDE rule for identifying outlier lesions [9].
Understanding how doctors check a mole for cancer removes a lot of the anxiety around the process. The appointment follows a logical, step-by-step approach: history review, visual examination, ABCDE assessment, and a decision about whether to monitor, biopsy, or remove. The exam itself is painless. If a biopsy is needed, local anesthetic makes the procedure comfortable for the vast majority of patients.
The single most important takeaway is this: visual assessment can identify suspicious moles, but pathology is the only way to confirm cancer. Waiting to "see if it changes" when a mole already shows warning signs is the most common and most avoidable mistake patients make.
Actionable next steps:
Skin cancer caught early is highly treatable. A 15-minute mole check can make a significant difference in outcomes.
[1] Screening - https://www.moffitt.org/cancers/melanoma/diagnosis/screening/
[2] Mole Mapping - https://www.aimatmelanoma.org/melanoma-101/early-detection-of-melanoma/mole-mapping/
[4] Skin Cancer Screening: What to Expect During a Dermatology Exam - https://www.dcsionline.com/blog/1431987-skin-cancer-screening-what-to-expect-during-a-dermatology-exam/
[5] Skin Cancer Screening - https://medlineplus.gov/lab-tests/skin-cancer-screening/
[6] SquareMind robotic mole scanning announcement - https://www.instagram.com/p/DXxW19_E8B1/
[7] Melanoma 2026 Cutting Edge Research and Predictions - https://www.theminorsurgerycenter.com/blog/melanoma-2026-cutting-edge-research-and-predictions
[8] ScienceDaily: AI melanoma risk prediction study - https://www.sciencedaily.com/releases/2026/04/260415043612.htm
[9] Screening Moles Cancer - https://www.webmd.com/melanoma-skin-cancer/screening-moles-cancer
[10] PMC review on dermoscopy and AI in melanoma detection - https://pmc.ncbi.nlm.nih.gov/articles/PMC12856975/
Last updated: May 12, 2026