Last updated: May 12, 2026
Quick Answer: A mole check is a clinical assessment to determine whether a mole appears benign, suspicious, irritated, or suitable for removal. Mole removal is a procedure that physically removes the mole from the skin. If a mole looks suspicious during a check, removal or biopsy may be recommended so the tissue can be tested by a pathology lab. These are two distinct steps — one is diagnostic, the other is surgical.
A mole check and mole removal are not the same thing, and confusing the two can delay important care. A mole check is a clinical assessment — a trained clinician examines your skin, evaluates individual moles, and decides whether any require further action. Mole removal is a separate procedure that physically takes the mole off your body.
Think of it this way: a mole check is the diagnosis step, and mole removal is the treatment step. One informs the other. For anyone wondering about mole check vs. mole removal: what is the difference?, the simplest answer is that a check tells you what you have, and removal addresses it if needed.
Both services are available at clinics like The Minor Surgery Center, which has performed over 9,000 mole procedures across Ontario.
A mole check is a structured skin examination performed by a doctor, nurse practitioner, or dermatologist to assess whether a mole or skin lesion is benign, suspicious, or in need of treatment.
During a mole check, the clinician will:
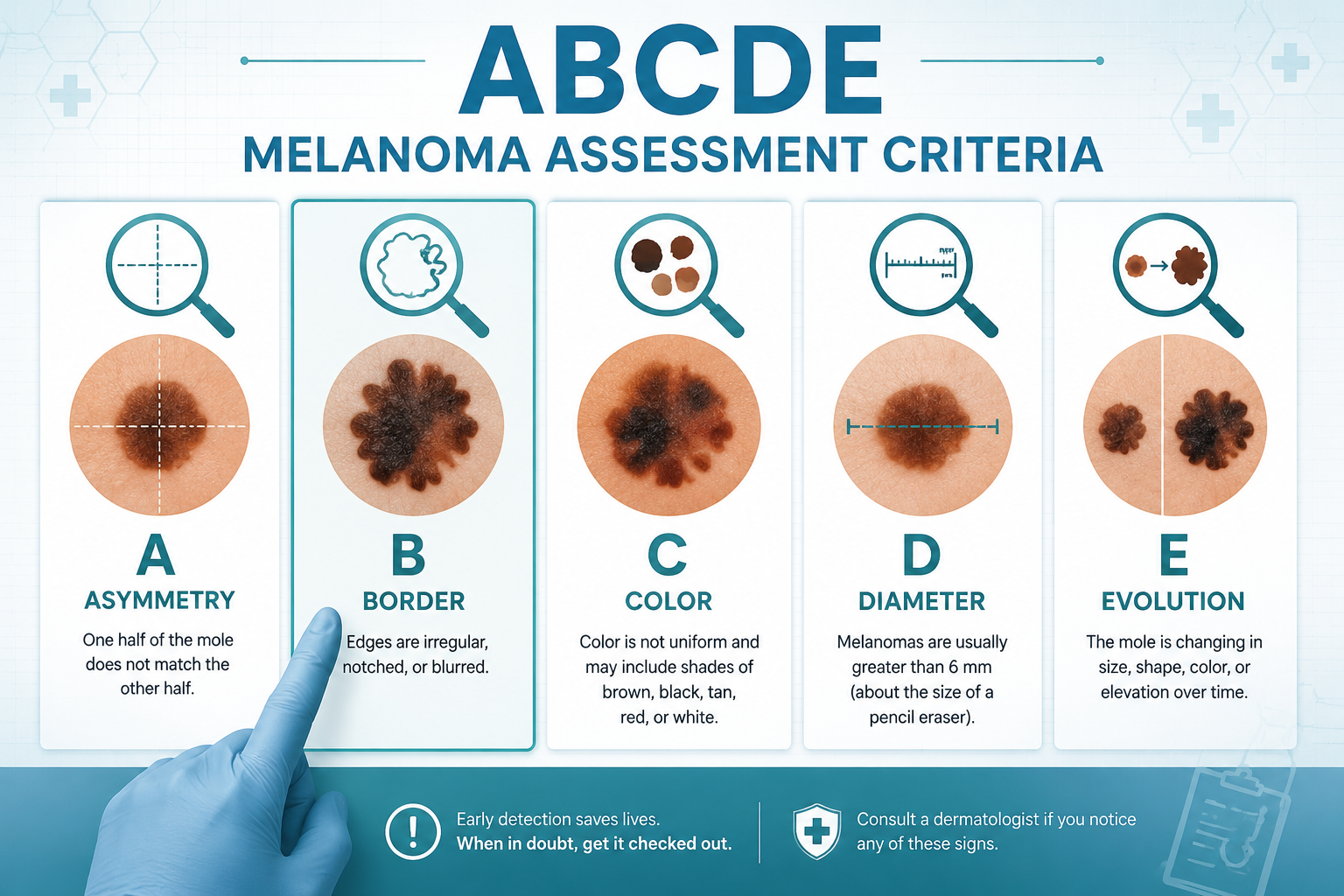
The ABCDE criteria are the standard framework clinicians use to evaluate moles:
LetterStands ForWhat to Look ForAAsymmetryOne half doesn't match the otherBBorderEdges are irregular, ragged, or blurredCColorMultiple shades of brown, black, red, white, or blueDDiameterLarger than 6mm (about the size of a pencil eraser)EEvolutionAny change in size, shape, color, or new symptoms
After the assessment, the clinician gives a recommendation: monitor the mole, schedule a follow-up, refer to a specialist, or proceed to removal or biopsy.
Mole mapping is a more advanced version of a mole check. It uses high-resolution photography and specialized software to create a digital record of all your moles, allowing clinicians to detect even subtle changes over time [3]. Standard mole checks provide real-time clinical assessment at a single visit, while mole mapping builds a longitudinal picture. For more on finding this service, see this guide to mole mapping clinics in Toronto.
💡 Key point: A mole check does not involve cutting, numbing, or any recovery time. It is a consultation and examination, not a procedure.
Mole removal is a minor surgical procedure in which a clinician physically removes a mole from the skin. It can be done for medical reasons (a suspicious or irritating mole) or cosmetic reasons (a mole the patient finds bothersome).
The three most common removal methods are:
The mole is shaved flush with the skin surface using a scalpel or razor blade. This method works well for raised, benign moles. It typically does not require stitches, heals relatively quickly, and leaves a minimal scar. To understand whether stitches are needed, see this guide on mole removal and stitches.
A circular punch tool removes a small, full-thickness core of skin. This is suited for smaller moles and usually requires one or two stitches. It allows the full mole, including deeper layers, to be sent for pathology.
The mole and a margin of surrounding skin are cut out in an elliptical shape, then the wound is closed with sutures. This is the preferred method for suspicious moles, larger lesions, or any case where complete removal with clear margins is important.
Plasma pen technology is also emerging as a non-invasive option for superficial moles, using plasma energy to vaporize tissue without cutting [7]. However, like laser removal, it does not preserve tissue for pathology — which limits its use for anything suspicious.
Patients considering cosmetic removal can learn more about the cosmetic mole removal process and what to expect.
Any mole that is new, changing, or causing symptoms should be assessed by a clinician before any decision is made about removal. Skipping the check and going straight to removal — especially with a non-surgical method — risks missing a diagnosis.
Specific situations that call for a mole check include:
As Mayo Clinic's Dr. Degesys notes, "Any mole that's increasing in size or evolving in any way, such as color, size or shape, or new symptoms should be examined." [4]
A check is also appropriate for anyone with a personal or family history of melanoma, significant sun exposure history, or a large number of moles. Banner Health recommends regular skin self-exams and professional checks as part of routine skin health monitoring [1].
A mole needs to be removed when it is suspicious for malignancy, causing physical irritation, or when the patient wants it gone for cosmetic reasons — provided a clinician has confirmed it is safe to remove.
Common reasons for mole removal include:
Not every suspicious mole is automatically removed. Some are monitored with repeat checks or mole mapping, especially if they are mildly atypical. The decision depends on the mole's appearance, the patient's risk profile, and clinical judgment [8].
Patients in the GTA can access removal services at multiple locations, including Downtown Toronto, Mississauga, Oakville, and Markham.
A mole biopsy means tissue is removed and sent to a pathology lab for microscopic analysis. Mole removal means the entire mole is excised, but it may or may not include pathology testing. The important distinction is what happens to the tissue after it leaves your body.
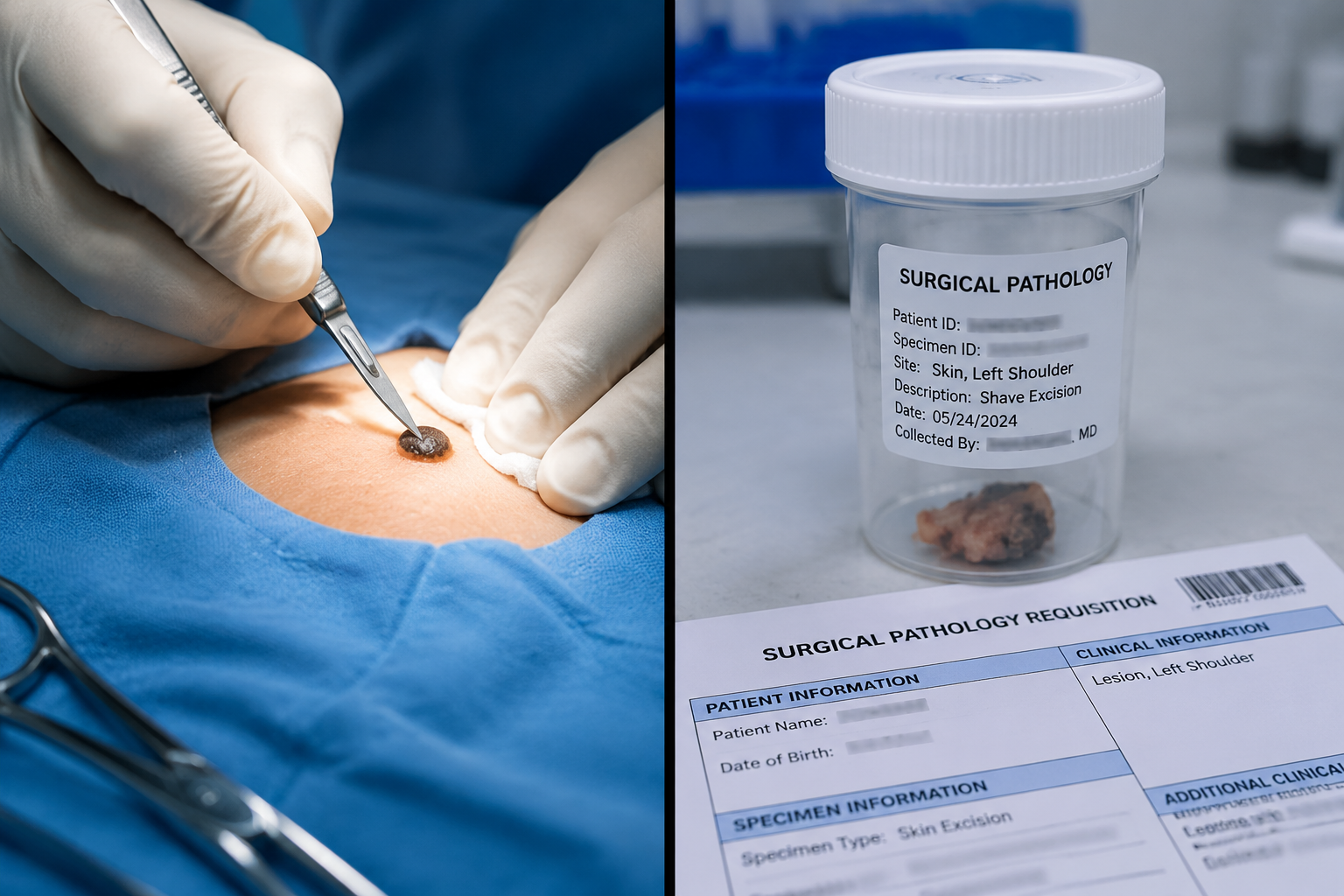
Here is how the two concepts overlap and differ:
Mole BiopsyMole RemovalTissue removed?Yes (partial or full)Yes (full mole)Sent to pathology?AlwaysSometimes (clinician's discretion)PurposeDiagnosisDiagnosis and/or cosmetic/medical treatmentMethodsShave, punch, or excisionalShave, punch, excision, laser, radiofrequencyLeaves a scar?Small scar possibleSmall scar possible
The same procedure can accomplish both goals. For example, a punch excision can completely remove a small mole and simultaneously send the tissue to pathology. In that case, the procedure is both a removal and a biopsy.
When a clinician removes a mole and sends it to a lab, you receive a pathology report that confirms whether the tissue is benign, dysplastic, or malignant. Understanding that report is important — this guide to reading your pathology report after mole removal walks through what the results mean.
Edge case: If a clinician removes a mole without sending it to pathology (common for clearly benign cosmetic removals), there is no tissue-based confirmation of the diagnosis. For any mole with uncertain features, pathology should always be requested.
Technically, some clinics offer removal without a prior formal check, but this is not best practice — especially for pigmented, changing, or irregular moles. A clinical assessment before removal protects the patient and the clinician.
Here is why the check matters:
A qualified clinician will always assess a mole before recommending a removal method. This is not just good practice — it is the standard of care for pigmented lesions [8].
Choose removal without a prior check only if: the mole has been previously assessed and documented as benign, and you are returning to have it removed for cosmetic reasons with no new changes.
Laser mole removal is not appropriate for moles that are suspicious for malignancy. The reason is straightforward: laser energy vaporizes tissue, which means there is nothing left to send to a pathology lab.
For clearly benign, superficial moles, laser treatment can be an effective cosmetic option with minimal scarring and fast recovery. But the moment a mole raises any clinical concern, tissue analysis becomes essential.
Key points on laser vs. surgical removal:
A 2026 analysis from Dr. Ardesh confirms that larger, deeper moles require surgical removal for complete excision and tissue analysis, while superficial moles are better candidates for laser treatment.
⚠️ Important: If a clinician or clinic offers laser removal for a mole you have not had assessed, ask why tissue analysis is not being recommended. For any pigmented or changing mole, insist on a clinical assessment first.
Melanoma cases are projected to continue rising in 2026 [9], which makes appropriate diagnostic steps before any removal procedure more important than ever.
Start with a mole check if you are unsure about any mole. Proceed to removal only after a clinician has assessed the mole and recommended it.
Use this framework to decide your next step:
Book a mole check if:
Book a removal consultation if:
Use the minor surgery cost estimator to get an idea of what removal may cost before your consultation.
The Minor Surgery Center offers consultations across Ontario, including Brampton, North York, Newmarket, and many other locations. Book a consultation to get a professional assessment and clear recommendation.
A mole check is a clinical examination to assess whether a mole is benign, suspicious, or needs treatment. Mole removal is a minor surgical procedure that physically excises the mole. A check comes first; removal follows if indicated.
Yes, for any pigmented, changing, or irregular mole, a clinical assessment should happen before removal. The check determines which removal method is appropriate and whether pathology is needed. Skipping this step can delay a cancer diagnosis.
A mole should be removed when it is suspicious for malignancy, confirmed as dysplastic, causing physical irritation, or when the patient wants it removed for cosmetic reasons after a clinician has confirmed it is safe to do so [8].
No. Some mildly atypical moles are monitored with repeat checks or mole mapping rather than removed immediately. The decision depends on the degree of concern, the patient's risk factors, and the clinician's judgment.
A biopsy means tissue is taken and sent to a pathology lab for testing. Removal means the mole is excised from the skin. These can happen in the same procedure — for example, a surgical excision that removes the mole and sends the tissue to pathology simultaneously.
Yes, if the removed tissue is sent to a pathology lab. Surgical excision and punch excision both preserve tissue for analysis. Laser and radiofrequency ablation do not, because the tissue is destroyed during the procedure.
No. Laser removal vaporizes tissue, leaving nothing for pathology testing. Suspicious moles require surgical removal so the tissue can be analyzed for malignancy. Laser is only appropriate for confirmed benign, superficial lesions [10].
No. Removing a mole does not cause cancer. This is a common misconception. If a mole contains cancerous or precancerous cells, removing it with adequate margins is part of treatment, not a cause of spread. For more detail, see this article on whether mole removal causes cancer.
It is possible, though uncommon with complete excision. If mole cells remain at the base after a shave excision, the mole may partially regrow. Complete surgical excision significantly reduces this risk. Learn more about mole regrowth after removal.
All skin procedures leave some degree of scarring, but the size and visibility of the scar depend on the removal method, the mole's location, and aftercare. Shave excisions typically leave the smallest marks. Proper scar care — including silicone gel and sun protection — improves outcomes significantly.
The distinction between a mole check and mole removal is not just semantic — it has real clinical consequences. A check is a diagnostic step that tells you what you are dealing with. Removal is a treatment step that addresses it. Doing them in the right order protects your health and ensures the right method is used.
Actionable next steps:
Early detection of melanoma is consistently associated with significantly better outcomes [PubMed, 2023]. A mole check costs very little time. Delaying one can cost much more.
[1] Moles - https://www.bannerhealth.com/services/dermatology/moles
[3] Difference Between Mole Mapping Vs Mole Check - https://dermasurge.co.uk/difference-between-mole-mapping-vs-mole-check/
[4] How Often Should I Get Moles Checked - https://mcpress.mayoclinic.org/living-well/how-often-should-i-get-moles-checked/
[7] Is Mole Removal Still Popular In 2026 - https://www.medicalcenterturkey.com/is-mole-removal-still-popular-in-2026/
[8] When Should You Consider Mole Removal - https://www.mohssurgerymd.com/blog/when-should-you-consider-mole-removal
[9] Melanoma Cases Projected Increase 2026 - https://www.medscape.com/viewarticle/melanoma-cases-projected-increase-2026-2026a10002dw
[10] Erbium Laser Vs Radiofrequency Mole Removal Which Treatment Is Best For You - https://moleremovalsanfrancisco.com/erbium-laser-vs-radiofrequency-mole-removal-which-treatment-is-best-for-you/