Quick Answer: A nerve conduction study (NCS) combined with electromyography (EMG) is a two-part electrodiagnostic test that measures how well your nerves and muscles communicate electrical signals. In Ontario, NCS/EMG is covered by OHIP when ordered by a physician, meaning most eligible patients pay nothing out of pocket. The test typically takes 45 minutes to 2 hours, is performed by a specialist neurologist or physiatrist, and results are usually discussed with you the same day [7].
A nerve conduction study (NCS) measures the speed and strength of electrical signals traveling through your peripheral nerves. EMG (electromyography) measures the electrical activity inside individual muscles. Together, they form the standard electrodiagnostic workup for nerve and muscle disorders [1].
How the two parts differ:
ComponentWhat It TestsHow It's DoneNCS (Nerve Conduction Study)Nerve signal speed and amplitudeElectrodes placed on skin; small electrical pulses appliedEMG (Electromyography)Muscle electrical activity at rest and during contractionFine needle electrode inserted into specific muscles
The NCS portion feels like a brief, mild electrical pulse — similar to a small static shock. The EMG needle causes brief discomfort when inserted, but most patients describe it as tolerable, not painful. London Health Sciences Centre (LHSC), which performs over 3,000 NCS/EMG studies per year, reports that the vast majority of patients tolerate the test well [7].
Common mistake: Many patients assume "EMG" and "NCS" are the same test. They are complementary but distinct. Your physician may order one or both depending on your symptoms.
NCS/EMG is ordered when a physician suspects a problem with the peripheral nervous system — the nerves outside the brain and spinal cord — or with the muscles themselves [1].
Typical reasons for referral include:
Choose NCS/EMG if: You have localized nerve symptoms and your physician needs to confirm the location, severity, and type of nerve injury before recommending treatment or surgery.
NCS/EMG may not be the right first step if: Your symptoms are primarily structural (e.g., a visible disc herniation on imaging) and the clinical picture is already clear. In those cases, MRI may be ordered first [10].
Clinical note: NCS/EMG is particularly valuable for distinguishing between carpal tunnel syndrome and cervical radiculopathy — two conditions that can cause nearly identical hand symptoms but require very different treatments.
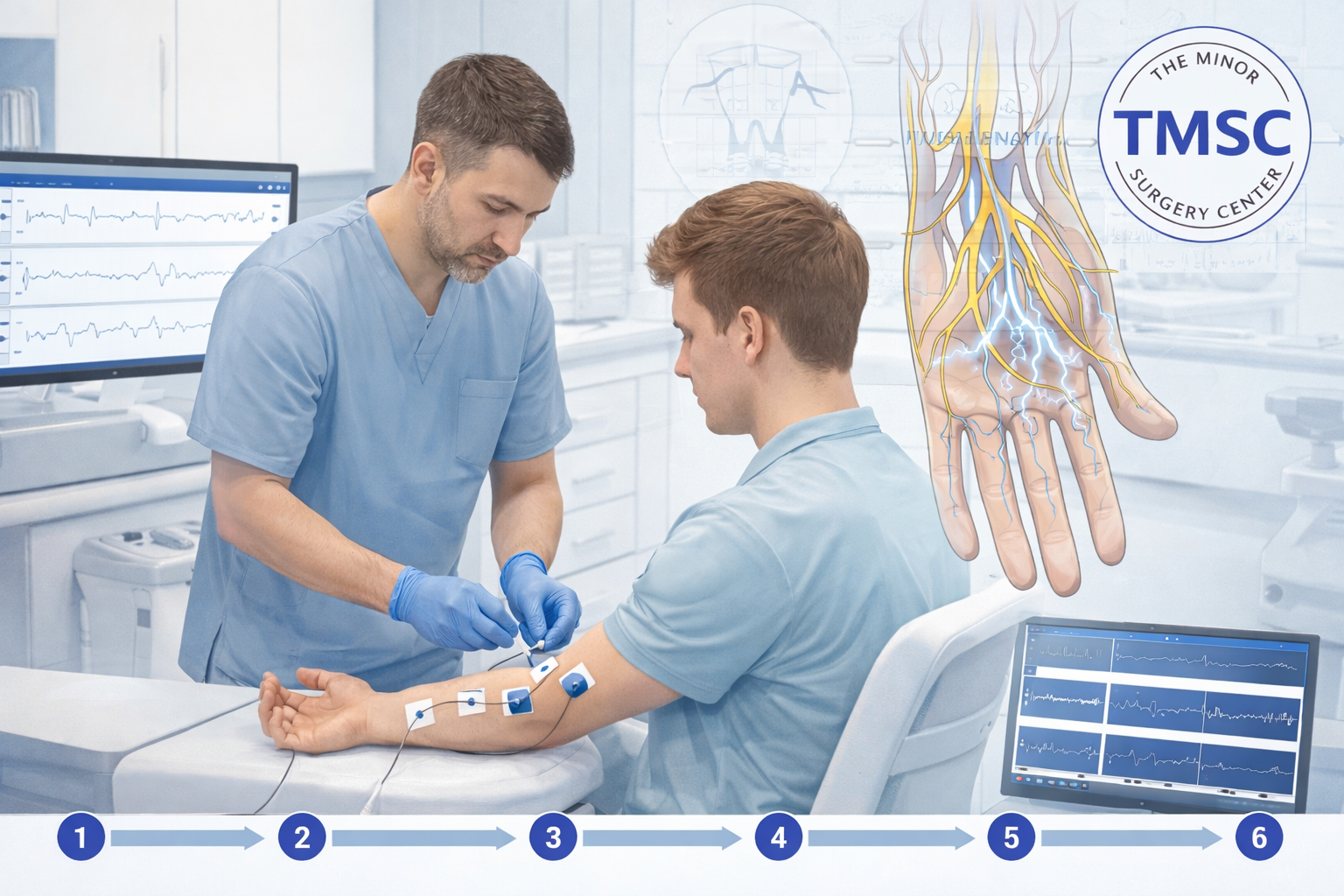
Here is exactly what happens from the moment you arrive at an Ontario EMG lab to when you leave with your results [7][5].
Step 1 — Patient history review
The performing physician (neurologist, physiatrist, or CSCN-certified specialist) reviews your symptoms and the reason for referral before beginning [7].
Step 2 — Nerve Conduction Study (NCS)
Small adhesive electrodes are placed on the skin over the nerve being tested. A stimulating electrode delivers a mild electrical pulse. You feel a brief, sharp sensation — most patients describe it as a small "zap." The machine records how fast and how strongly the signal travels [1][3].
Step 3 — Electromyography (EMG)
A thin needle electrode is inserted into specific muscles. You will be asked to relax, then contract the muscle at varying levels. The needle records the electrical patterns. There may be brief discomfort during insertion, but the needle does not inject anything [1][4].
Step 4 — Real-time analysis
The physician reviews the waveforms as the test progresses and may adjust which nerves or muscles are tested based on findings [7].
Step 5 — Results discussion
In most Ontario EMG labs, the physician discusses preliminary findings with you before you leave. A formal written report is sent to your referring physician [7].
Appointment duration: 45 minutes for simple single-nerve studies; up to 2 hours for complex cases involving multiple limbs or suspected myopathy [7].
For most Ontario residents, the out-of-pocket cost for an OHIP-covered NCS/EMG is $0. OHIP reimburses the performing physician directly, and patients are not billed for insured services [6].
OHIP billing context: The OHIP Fee Schedule includes specific codes for electrodiagnostic studies. A limited NCS study (single nerve) was billed at approximately $61.95 under the pre-2026 schedule (code G457). The April 1, 2026 OHIP Fee Schedule update introduced fee increases of approximately 10–14% across specialties, which would affect electrodiagnostic billing rates, though no electrodiagnostic-specific code changes were announced [6].
Important: Clinics that accept OHIP for NCS/EMG cannot charge patients an additional private fee for the same insured service. If a clinic quotes you a private fee for an OHIP-eligible study, ask for clarification before proceeding.
Some situations fall outside OHIP coverage — for example, non-residents, patients without a valid referral, or studies ordered for insurance or legal purposes. In those cases:
ScenarioEstimated Cost (CAD)Single nerve NCS (private)$150–$350 (estimated)Full NCS/EMG study (private)$400–$800+ (estimated)U.S. outpatient EMG benchmark~$500 USD (2025 data)
Note: Private pricing varies significantly by clinic and region. These are estimates only — confirm directly with the clinic.

Preliminary findings are typically discussed on the day of the test. The formal written report is sent to your referring physician within a few days to two weeks, depending on the lab's volume and workflow [7].
What the report includes:
Edge case: If the results are unexpected or complex (e.g., findings suggest a rare neuromuscular disease), the EMG physician may contact your referring physician directly before the formal report is sent.
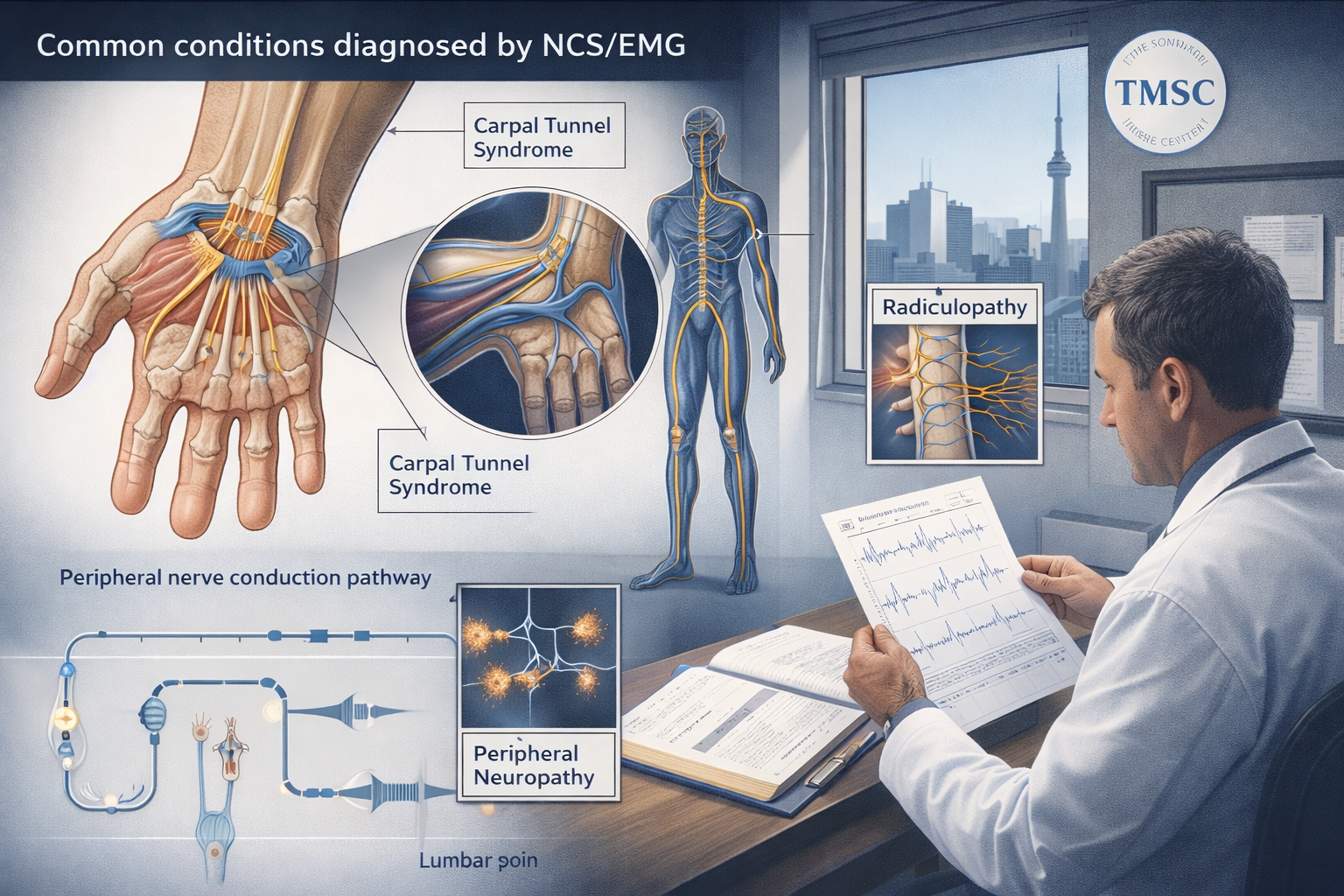
NCS/EMG is the primary diagnostic tool for a wide range of peripheral nerve and muscle disorders [1][10].
Nerve disorders:
Muscle disorders (myopathies):
Neuromuscular junction disorders:
What NCS/EMG cannot reliably detect:
Clinical pearl: A normal NCS/EMG does not rule out all nerve problems. If symptoms persist despite a normal study, discuss small-fiber neuropathy testing or repeat electrodiagnostics with your physician.
If you've been experiencing hand numbness and are unsure whether your symptoms point to carpal tunnel or something else, reviewing the common misdiagnoses in carpal tunnel syndrome can help you ask better questions at your appointment.
NCS/EMG is not the only tool available. The right test depends on what your physician is looking for [10].
TestBest ForLimitationNCS/EMGLocalizing nerve dysfunction, assessing severity, diagnosing myopathyCannot visualize structural anatomy; misses small-fiber neuropathyMRIVisualizing disc herniation, nerve root compression, structural lesionsDoes not measure nerve function; expensive, longer waitUltrasoundVisualizing nerve swelling, entrapment sites in real timeOperator-dependent; limited functional informationCT scanBony structural abnormalitiesRadiation exposure; poor soft tissue resolution
Choose NCS/EMG if: You need functional information — how well the nerve is conducting, whether the muscle is denervated, and where exactly the lesion is located.
Choose MRI if: The clinical picture strongly suggests a structural cause (e.g., disc herniation with clear dermatomal pattern) and surgery is being considered.
Both together: For complex cases like brachial plexopathy or suspected cervical myelopathy, NCS/EMG and MRI are often ordered together for a complete picture.
For patients already diagnosed with carpal tunnel syndrome and exploring non-surgical options, resources on carpal tunnel stretches and nerve glides and advances in carpal tunnel syndrome management provide useful context before deciding on next steps.
Getting an NCS/EMG in Ontario requires a physician referral. Here is how the process works in practice.
Ontario regulatory note: As of January 1, 2026, Ontario expanded "As of Right" rules to 16 health professions, streamlining recognition for physicians moving between provinces. This may modestly improve availability of qualified EMG physicians in underserved regions, though it does not directly change the NCS/EMG procedure itself [9].
If you are in the Greater Toronto Area and looking for expedited specialist access with board-certified physicians, The Minor Surgery Center's carpal tunnel surgery program offers consultations without long public system wait times for patients who have already received their NCS/EMG diagnosis.
Q: Does an NCS/EMG hurt?
The NCS portion causes brief, mild electrical pulses — most patients describe it as a small shock or snap. The EMG needle causes brief discomfort when inserted into muscle, but most patients tolerate it well. LHSC reports that the test is well-tolerated by the vast majority of its 3,000+ annual patients [7].
Q: Do I need a referral for NCS/EMG in Ontario?
Yes. OHIP coverage requires a physician referral. Without one, you would need to pay privately, which is uncommon for this test.
Q: How long does the test take?
Between 45 minutes and 2 hours, depending on how many nerves and muscles are tested [7].
Q: Can I drive myself home after an NCS/EMG?
Yes. There are no sedatives involved, and there are no restrictions on driving or activity after the test [5].
Q: Will the results tell me if I need surgery?
NCS/EMG results inform the clinical decision, but surgery is not decided based on the test alone. Your physician will combine the electrodiagnostic findings with your symptoms, physical examination, and imaging before recommending surgery. For carpal tunnel, for example, moderate-to-severe NCS findings often support surgical referral.
Q: What if my NCS/EMG is normal but I still have symptoms?
A normal result does not rule out all nerve conditions. Small-fiber neuropathy, for example, is not detected by standard NCS/EMG [10]. Discuss further testing options — including skin punch biopsy or autonomic studies — with your physician.
Q: How often can I have an NCS/EMG?
There is no strict limit. Repeat studies are sometimes ordered to monitor disease progression or recovery after treatment. OHIP covers repeat studies when clinically indicated.
Q: Is NCS/EMG safe during pregnancy?
The test is generally considered safe during pregnancy, as it uses only small electrical pulses and needle insertion — no radiation or contrast agents. Discuss with your obstetrician and the performing physician if you are pregnant.
Q: What is a CSCN Diplomate?
The Canadian Society of Clinical Neurophysiologists (CSCN) offers certification for physicians who have completed specialized training in electrodiagnostic medicine. CSCN Diplomate status indicates advanced competency in NCS/EMG interpretation [7][2].
Q: Can a chiropractor order an NCS/EMG in Ontario?
As of 2026, chiropractors in Ontario cannot directly order NCS/EMG studies. Proposed scope expansions announced in September 2025 may eventually allow chiropractors to order advanced diagnostics, but electrodiagnostic ordering authority has not been extended to chiropractors as of this writing.
Q: What happens if the EMG shows denervation?
Denervation on EMG means a muscle is not receiving normal nerve signals — it indicates active nerve damage. The clinical significance depends on the pattern, location, and severity. Your physician will interpret this in the context of your full clinical picture and may recommend further imaging, specialist referral, or surgical consultation.
Q: Is there anything I should avoid before the test?
Avoid applying lotions, creams, or oils to your skin on the day of the test. Wear loose clothing. Do not stop medications without physician guidance. Caffeine and food are generally fine [5].
A nerve conduction study (NCS/EMG) in Ontario is one of the most informative diagnostic tools available for evaluating peripheral nerve and muscle disorders. For the majority of Ontario residents, the test is covered by OHIP at no direct cost, takes under two hours, and provides same-day preliminary results from a qualified specialist.
Understanding what to expect — from the referral process to the needle insertion to the post-test report — reduces anxiety and helps patients engage more effectively with their care team. The test is not perfect: it can miss small-fiber neuropathy and very early nerve injuries, so clinical correlation always matters.
Actionable next steps:
Expedited, specialist-led care is available. The right diagnosis is the first step toward the right treatment.
[1] Electromyography EMG And Nerve Conduction Studies - https://medlineplus.gov/lab-tests/electromyography-emg-and-nerve-conduction-studies/
[2] Watch - https://www.youtube.com/watch?v=GalU9SWiYic
[3] Nerve Conduction Study - https://www.upmc.com/services/spine/services/tests/nerve-conduction-study
[4] What To Expect During An EMG/NCS - https://www.kcbj.com/blog/what-to-expect-during-an-emgncs-29735/
[5] EMG What To Expect - https://centers.rowanmedicine.com/nmi/documents/emg_whattoexpect.pdf
[6] OHIP Billing Codes - https://opsmed.ca/ohip-billing-codes/
[7] What To Expect During Your EMG Test - https://www.lhsc.on.ca/emg-lab/what-to-expect-during-your-emg-test
[9] Ontario "As of Right" Expansion - https://www.facebook.com/SylviaJonesMPP/posts/as-of-jan-1-2026-our-government-is-expanding-as-of-right-rules-to-16-additional-/1325000116104708/
[10] EMG And Nerve Conduction Studies - https://davydhooper.com/nerve-and-muscle-diseases/emg-and-nerve-conduction-studies/
Last updated: April 28, 2026