Last updated: March 5, 2026
Most skin cancers are caught early because someone noticed a change. But melanoma and other skin cancers don't only appear on easy-to-see spots like the arms or face. They grow in places most people never think to check: under the hair, down the back, behind the ears, beneath the nails, and on the soles of the feet. Knowing how to check hard-to-see areas — scalp, back, ears, nails, and soles — can genuinely make the difference between catching something early and missing it until it's advanced.
This guide covers exactly how to examine each of these hidden zones, what warning signs to look for, and when to get a professional involved.
To check hard-to-see areas — scalp, back, ears, nails, and soles — use a combination of a full-length mirror, a handheld mirror, good lighting, and ideally a partner. Part the scalp section by section with a comb, use two mirrors for the back, inspect the nail beds for dark streaks, and examine the soles and between the toes after bathing. Any lesion that is asymmetric, has irregular borders, shows multiple colors, is larger than 6mm, or is changing over time should be evaluated by a doctor. [1][7]
Skin cancer found early is highly treatable. The challenge is that the body's most vulnerable zones are often the ones people skip during self-exams.
The scalp, back, ears, nails, and soles share one thing: they're anatomically awkward to inspect without tools or help. As a result, lesions in these areas tend to be diagnosed later, when treatment is more complex.
Key facts about hidden-area skin cancers:
"Performing a monthly skin self-exam is one of the most important things you can do for early detection." — Skin Cancer Foundation [1]
Understanding the first stages of skin cancer and what early lesions look like is the foundation before starting any self-exam routine.
Before examining hard-to-see areas, gather the right tools. A self-exam done without proper equipment misses the point.
Recommended tools:
ToolPurposeFull-length mirrorFull body overview, front and backHandheld mirrorScalp, back, ears, solesBlow dryerParting scalp hair section by sectionComb or fine-tooth pickSeparating hair for scalp checksBright, natural or LED lightAccurate color assessmentPartner (optional but helpful)Back, scalp, behind earsSmartphone cameraPhotographing lesions for tracking
Common mistake: Using dim bathroom lighting. Artificial incandescent bulbs can make pigmented lesions look lighter or darker than they are. Natural daylight or a bright LED lamp is more reliable for color accuracy.
The Skin Cancer Foundation recommends performing self-exams monthly, in a well-lit room, after a shower when skin is clean and dry. [1] Shady Grove Dermatology also advises noting the position, size, and color of any moles so changes can be tracked over time. [2]

This is the practical core of the guide. Each zone has its own technique.
The scalp is one of the hardest areas to self-examine, but a blow dryer and comb make it manageable. Part the hair in small sections, moving systematically from front to back and side to side.
Step-by-step scalp check:
What to look for on the scalp:
People with thick or dark hair may find partner checks especially useful. If there's a suspicious lesion on the scalp — particularly one that feels raised, bleeds easily, or has changed — review what a cancerous cyst on the scalp can look like, and consult a doctor promptly.
Edge case: Scalp psoriasis, seborrheic dermatitis, and epidermoid cysts can all mimic suspicious lesions. When in doubt, get it checked rather than self-diagnosing.
The back requires either two mirrors or a partner — there's no reliable way to examine it solo with just one mirror. This is the zone most commonly skipped in self-exams, and it's a high-risk site, especially for men.
Two-mirror technique for the back:
Partner check: Ask someone to systematically scan the entire back in good lighting, looking for new spots, moles that look different from others, or any raised or bleeding lesions.
Choose this approach if: You have a history of atypical moles or a family history of melanoma. In that case, partner checks every month are worth the effort. For a deeper look at what to watch for, see the guide on atypical moles.
Ear skin cancer is underdiagnosed because most people don't think to check the ear's many folds and surfaces. A handheld mirror and good lighting are all that's needed.
Areas to examine on and around the ear:
Technique: Hold a handheld mirror at an angle to reflect the ear in a larger mirror. Use a finger to gently fold back the ear rim to expose the skin underneath.
Squamous cell carcinoma is particularly common on the ear rim due to chronic sun exposure. For context on what squamous cell lesions look like, the guide on cutaneous squamous cell carcinoma is a useful reference.
Note: Cysts behind the ear are common and usually benign, but any lump that grows, bleeds, or changes should be evaluated. See more on cysts behind the ear for comparison.
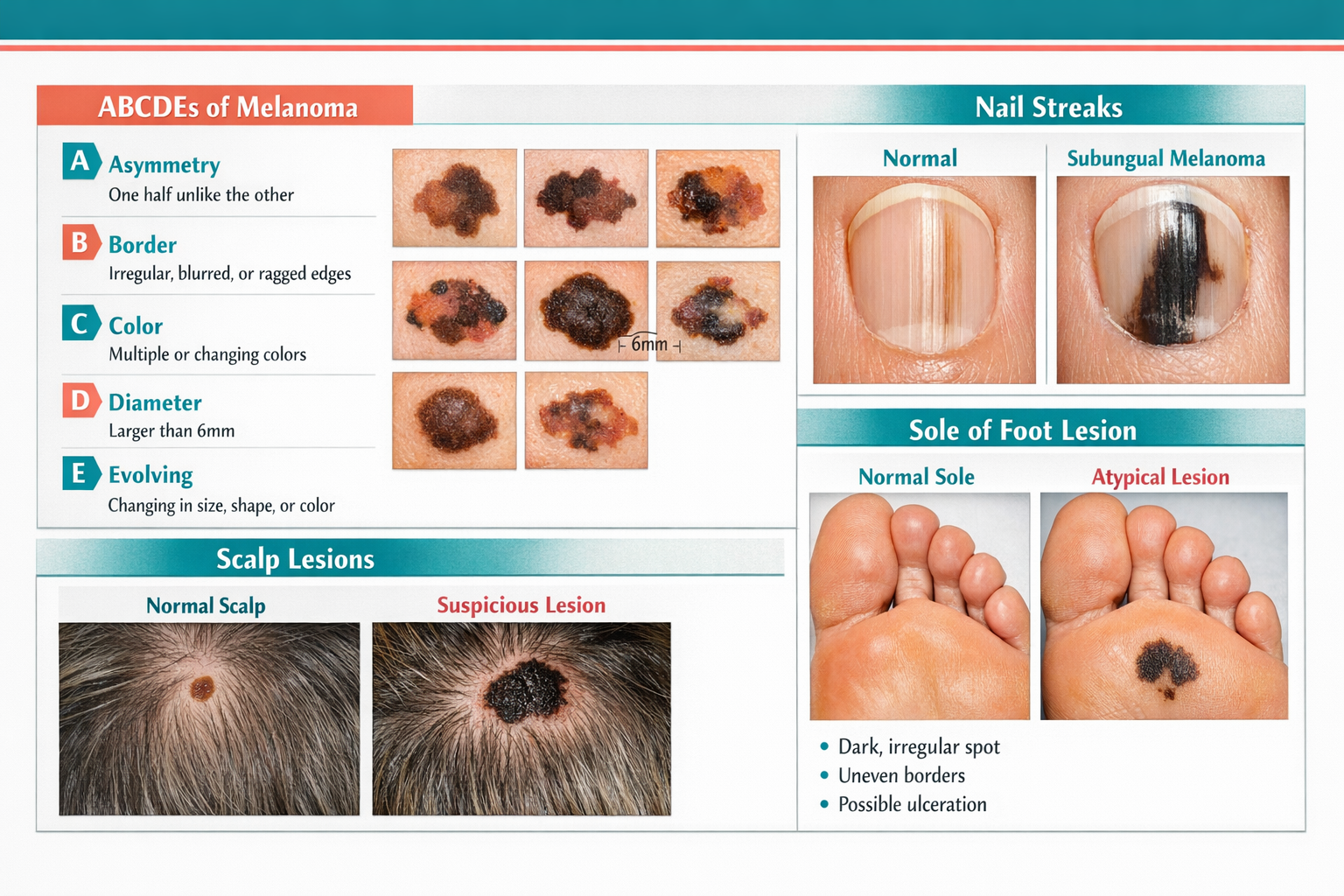
Nail melanoma signs include a dark vertical streak (called a longitudinal melanonychia) running from the base to the tip of the nail. This is the most important warning sign for subungual melanoma, and it's frequently dismissed as a bruise or fungal infection.
How to examine nails:
Nail melanoma warning signs:
SignDescriptionDark vertical streakBrown or black band running lengthwiseHutchinson's signPigment spreading from nail onto surrounding skinNail distortionNail lifting, splitting, or thickening without injuryNon-healing lesionSore at the nail fold that won't resolveRapid changeStreak widening or darkening over weeks
Important distinction: A single dark streak that appears suddenly, widens, or involves the thumb or big toe deserves urgent evaluation. Multiple pale streaks on several nails are more likely benign (common in darker skin tones, pregnancy, or certain medications).
Nail changes can also result from contact dermatitis. The article on contact dermatitis of the nails helps distinguish inflammatory from potentially malignant nail changes.
Common mistake: Assuming a dark streak under the nail is a bruise from footwear. A true subungual hematoma (bruise) usually grows out with the nail over weeks. A melanoma streak does not move.
Melanoma on the soles of the feet and between the toes is called acral lentiginous melanoma, and it's often caught late because people rarely look at the bottoms of their feet. Roswell Park Comprehensive Cancer Center recommends sitting down after a bath or shower to examine the soles, toenails, and the skin between each toe. [3]
How to check the soles:
What to look for:
For a detailed look at what early melanoma on the foot looks like, the article on early melanoma on the bottom of the foot provides visual context and clinical detail.
Who this matters most for: Acral lentiginous melanoma affects all skin tones but represents a higher proportion of melanoma diagnoses in people with darker skin. It's not caused by sun exposure, so standard UV-focused prevention messaging doesn't always prompt awareness of this subtype. [10]
The ABCDE rule works for every body site, including the scalp, nails, and soles. [7] Apply it the same way regardless of location.
LetterStands ForWhat to Look ForAAsymmetryOne half doesn't match the otherBBorderRagged, notched, or blurred edgesCColorMultiple shades of brown, black, red, white, or blueDDiameterLarger than 6mm (about the size of a pencil eraser)EEvolvingAny change in size, shape, color, or symptoms
Key point: "E for Evolving" is often the most important criterion in hidden areas. A lesion that has changed — even if it doesn't meet the other criteria — warrants professional evaluation. [7]
For nails specifically, the "E" criterion is critical: a streak that is widening, darkening, or developing Hutchinson's sign is evolving and needs prompt attention.
Emerging tools are making it easier to document and analyze hard-to-see areas, though none replace a professional exam.
Current options in 2026:
Smartphone apps: Apps like Miiskin and SkinVision allow users to photograph lesions over time and track changes. A February 2026 prospective study (NCT05246163) found that an AI smartphone app achieved 82.5% sensitivity and 76.8% specificity on real-world user photos of concerning lesions. That's useful for tracking, but it means roughly 1 in 6 melanomas could be missed by the app alone.
Wearable patch technology: Researchers at Wake Forest University School of Medicine developed a battery-free wearable patch (announced October 2025) that uses bioimpedance to detect abnormal skin tissue, distinguishing cancerous from healthy skin. In a 10-volunteer study, it worked wirelessly and was designed for at-home use, including hard-to-reach areas. This technology is still in early research stages.
AI-assisted clinical devices: The DermaSensor device (FDA-cleared) uses AI to analyze lesions and achieved 96% sensitivity across 224 cancers in a 1,000-patient study. [9] It's currently a clinical tool used by healthcare providers, not a consumer device, but it's increasingly available at dermatology offices and can help examine areas like the scalp or back during a professional visit.
Fox Chase Cancer Center announced an AI tool in October 2025 (MST-AI) designed to improve detection accuracy across all skin tones by correcting dataset imbalances — an important step given that acral melanoma in darker skin tones has historically been underrepresented in AI training data. [4]
Practical takeaway: Use apps to photograph and track lesions in hard-to-see areas between professional visits. Don't rely on an app result alone to rule out a concerning lesion. For a realistic look at what these tools can and can't do, see the article on whether 3D mole mapping apps are reliable.
Monthly self-exams of all body areas, including the scalp, back, ears, nails, and soles, are recommended by the Skin Cancer Foundation. Annual professional skin exams are also advised, particularly for people with risk factors. [1][8]
Self-exam frequency:
See a doctor promptly if:
Annual professional exams are especially important for people who can't easily self-examine (limited mobility, visual impairment, thick hair). The Skin Cancer Foundation notes that a dermatologist can examine areas that are genuinely inaccessible to self-check. [8]
For those in the Toronto and surrounding area, finding a melanoma oncologist near you is a practical next step if a concerning lesion is found.
Knowing how to check hard-to-see areas — scalp, back, ears, nails, and soles — also means knowing what goes wrong during self-exams.
Mistake 1: Skipping nail polish removal
Nail polish, especially dark colors, completely obscures the nail bed. Always remove polish before a nail check.
Mistake 2: Only checking moles, not all skin
Melanoma and squamous cell carcinoma can arise on skin with no pre-existing mole. Check all skin, not just existing spots.
Mistake 3: Checking in poor lighting
Dim or warm-toned lighting distorts color. Use bright, neutral-toned LED lighting or natural daylight.
Mistake 4: Assuming the scalp is protected by hair
Hair does not block UV radiation completely, especially on the part line or crown. The scalp is a legitimate high-risk zone. [1]
Mistake 5: Confusing a bruise under the nail with a streak
A subungual hematoma moves with nail growth (roughly 1mm per week for fingernails). A melanoma streak stays fixed at the nail matrix. If a dark area under the nail hasn't moved after 6–8 weeks, it needs evaluation.
Mistake 6: Waiting for symptoms
Most early skin cancers are painless. Waiting for a lesion to hurt or bleed means waiting too long.
Q: Can melanoma grow on the scalp even if I wear a hat?
Yes. Hats reduce UV exposure but don't eliminate it. Melanoma can also develop on the scalp from causes other than UV radiation. Scalp melanoma is a real risk regardless of sun habits. [1]
Q: What does nail melanoma look like in early stages?
Early nail melanoma typically appears as a single dark brown or black vertical streak running from the base to the tip of one nail. It may be narrow at first. The key warning sign is that it widens, darkens, or spreads onto the surrounding skin (Hutchinson's sign).
Q: How do I check my own back without a partner?
Use a full-length mirror and a handheld mirror together. Stand with your back to the full-length mirror, hold the handheld mirror in front of you, and angle it to see your back's reflection. It takes practice but covers most of the back. A smartphone on a timer or tripod can also help photograph areas that are hard to angle mirrors toward.
Q: Is melanoma on the sole of the foot related to sun exposure?
No. Acral lentiginous melanoma, which appears on palms, soles, and under nails, is not caused by UV radiation. Its exact cause is not fully understood. This is why sunscreen use alone doesn't prevent this type of melanoma. [10]
Q: How is a dark streak under the nail different from a fungal nail infection?
Fungal nail infections typically cause yellowing, thickening, crumbling, or white patches — not a dark vertical streak. A dark streak that runs from the base of the nail to the tip is more characteristic of melanoma or benign melanocytic activation. When in doubt, see a doctor.
Q: Can children get melanoma in these hidden areas?
Melanoma is rare in children but does occur, particularly in adolescents with a family history or many atypical moles. The same self-exam principles apply. Any concerning lesion in a child should be evaluated by a pediatric dermatologist.
Q: How accurate are AI apps for checking hard-to-see areas?
A 2026 prospective study found an AI skin app achieved 82.5% sensitivity and 76.8% specificity on user-submitted photos. That means some cancers will be missed. AI apps are useful for tracking changes over time but should not be used as a substitute for professional evaluation of suspicious lesions.
Q: What if I find something suspicious during a self-exam?
Photograph it, note when you first noticed it, and book an appointment with a dermatologist or physician promptly. Don't wait to see if it changes further — early evaluation is always better.
Q: Are there specific skin types that need to check soles and nails more carefully?
Yes. Acral lentiginous melanoma represents a higher proportion of melanoma cases in people with darker skin tones. Regular sole and nail checks are especially important for this group, even though overall melanoma rates may be lower. [10]
Q: How long does a thorough self-exam of all hard-to-see areas take?
A complete self-exam, including scalp, back, ears, nails, and soles, takes about 10–15 minutes when done properly. Monthly consistency matters more than speed.
Q: Should I photograph lesions in hard-to-see areas?
Yes. Photographing lesions with a smartphone and comparing images month to month is one of the most practical ways to detect the "E" (Evolving) criterion. Store photos with dates for reference at medical appointments.
Q: Can a GP (family doctor) check hard-to-see areas, or do I need a dermatologist?
A GP can perform a basic skin check and refer for concerning lesions. A dermatologist has specialized training and tools (including dermoscopy) for more accurate assessment. For any lesion that seems suspicious, a dermatologist referral is worth requesting.
Checking hard-to-see areas — scalp, back, ears, nails, and soles — is not complicated, but it does require the right tools, a consistent routine, and knowing what to look for. Most people skip these zones entirely, which is exactly why cancers there are often caught late.
Start here:
Early detection saves lives. The five minutes it takes to check the scalp, back, ears, nails, and soles each month is among the most useful health habits anyone can build.
[1] Self Exams - https://www.skincancer.org/early-detection/self-exams/
[2] How To Conduct A Mole Self Check Between Doctor Visits - https://www.shadygrovederm.com/post/how-to-conduct-a-mole-self-check-between-doctor-visits
[3] Skin Self Exam - https://www.roswellpark.org/cancer/skin/diagnosis/skin-self-exam
[4] Ai Powered Diagnostics - https://www.aimatmelanoma.org/ai-powered-diagnostics/
[5] MedlinePlus - https://medlineplus.gov/ency/patientinstructions/000711.htm
[7] ABCDEs Of Melanoma: How To Check Your Moles At Home - https://www.mdcsnyc.com/post/abcdes-of-melanoma-how-to-check-your-moles-at-home
[8] Annual Exams - https://www.skincancer.org/early-detection/annual-exams/
[9] FDA Clearance Granted For First AI-Powered Medical Device To Detect All Three Common Skin Cancers - https://www.dermasensor.com/resource/fda-clearance-granted-for-first-ai-powered-medical-device-to-detect-all-three-common-skin-cancers-melanoma-basal-cell-carcinoma-and-squamous-cell-carcinoma/
[10] NBK225245 - https://www.ncbi.nlm.nih.gov/books/NBK225245/