Last updated: January 15, 2026
A dark streak or spot under your nail can trigger immediate concern. Subungual melanoma, a rare but serious form of skin cancer that develops beneath the nail, shares visual similarities with common nail bruises (subungual hematomas), making accurate identification crucial for early intervention. This melanoma on nails (subungual) vs bruise: quick guide provides clear criteria to distinguish between these two conditions and explains when medical evaluation becomes necessary.
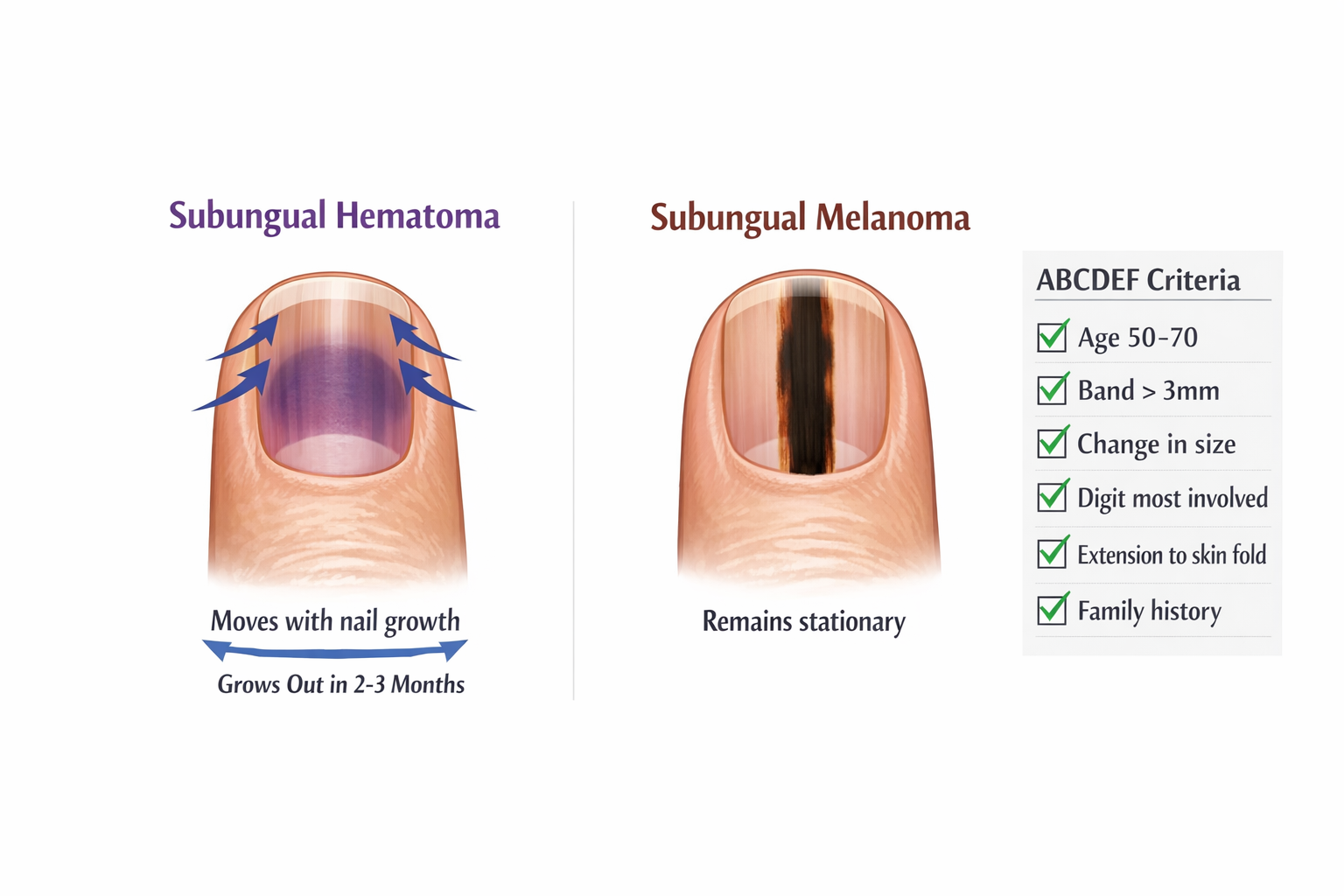
Subungual melanoma and nail bruises differ primarily in their behavior over time and appearance patterns. A bruise under the nail will gradually move toward the nail tip as the nail grows, typically resolving within 2-3 months for fingernails or up to 9 months for toenails. In contrast, subungual melanoma appears as a vertical dark band that remains in the same position on the nail bed, often widening or darkening over time. Melanoma typically presents as a brown-black streak approximately 3mm wide with irregular borders, while bruises show more uniform purple-red-brown discoloration that follows a recent injury.
Subungual melanoma is a rare type of skin cancer that develops in the nail matrix (the tissue beneath the nail that produces nail cells). This form of melanoma accounts for approximately 0.7-3.5% of all melanoma cases worldwide, with higher prevalence in populations with darker skin tones.[2]
The fundamental difference between subungual melanoma and a nail bruise lies in their origin and progression:
Subungual Hematoma (Bruise):
Subungual Melanoma:
In 75-90% of cases, subungual melanoma develops specifically on the big toe or thumb, with the index finger being the third most common location.[2] This concentration in specific digits forms part of the diagnostic ABCDEF criteria used by dermatologists. Bruises, conversely, can occur on any nail and frequently affect multiple nails simultaneously when trauma involves the hand or foot.
Subungual melanoma presents as a distinct vertical dark line resembling a marker stroke drawn from the cuticle toward the nail tip.[3][4] The pigmentation shows irregular borders and varying shades of blackish-brown within the band. Hematomas appear as more uniform dark discoloration resembling a bruise or smudge, without the characteristic linear vertical pattern.[3]
The most reliable method to distinguish between a bruise and melanoma involves observing the spot's behavior over time and evaluating specific visual characteristics. Several key factors help differentiate these conditions before seeking professional evaluation.
For bruises: Mark the proximal edge (closest to the cuticle) of the dark area with a pen on the nail surface. Over subsequent weeks, a bruise will maintain its distance from this mark as both the mark and the bruise move toward the nail tip together. The dark area gradually shifts away from the cuticle.
For melanoma: The pigmented band remains in the same position relative to the nail bed. If you mark the nail surface, the mark will grow outward while the dark band stays stationary at its origin point in the nail matrix.[1][2]
Fingernails grow approximately 3mm per month, while toenails grow about 1mm per month.[5] Based on these growth rates:
Medical professionals use the ABCDEF guidelines specifically developed for identifying subungual melanoma:[2]
A - Age and Race
B - Brown to Black Band
C - Change
D - Digit
E - Extension
F - Family or Personal History
Bruises from trauma typically cause immediate throbbing pain that gradually subsides over days to weeks. The pain intensity correlates with the severity of the initial injury.[3]
Subungual melanomas remain typically painless throughout their development.[3] Pain in a melanoma case usually indicates advanced disease with nail bed destruction or secondary infection.
Bruise indicators:
Melanoma warning signs:[1]
The ABCDEF rule provides a systematic framework for evaluating suspicious nail pigmentation. This mnemonic device helps both patients and healthcare providers identify features that warrant further investigation.
Age (A): Subungual melanoma typically affects individuals aged 60-70 years old, though it can occur at any age.[2][6] Younger patients with nail discoloration more commonly have benign causes, though age alone never excludes melanoma.
Band (B): The characteristic presentation involves a brown to black longitudinal band measuring 3mm or wider.[2] Bands narrower than 3mm may still represent melanoma, particularly if they demonstrate other concerning features. The border irregularity matters as much as width—melanoma bands typically show blurred, uneven edges rather than sharp demarcation.
Change (C): Any modification in size, shape, or color intensity raises concern. Melanomas tend to darken progressively and widen over months to years. Benign pigmented bands (melanonychia) typically remain stable. Document changes with dated photographs for accurate tracking.
Digit (D): The thumb, big toe, and index finger account for the vast majority of subungual melanoma cases.[2] While melanoma can develop under any nail, involvement of these specific digits increases suspicion, particularly when combined with other ABCDEF features.
Extension (E): Hutchinson's sign—the extension of brown-black pigmentation from the nail onto the adjacent proximal or lateral nail fold—strongly suggests malignancy.[1][2] This occurs when melanoma cells migrate beyond the nail matrix into surrounding skin. However, absence of Hutchinson's sign does not exclude melanoma, and some benign conditions can create similar appearances (pseudo-Hutchinson's sign).
Family history (F): A personal or family history of melanoma or dysplastic nevus syndrome increases risk. Patients with previous melanoma diagnoses require heightened vigilance for new pigmented lesions, including subungual presentations.
The ABCDEF criteria serve as a screening tool, not a diagnostic certainty. Some melanomas present without meeting all criteria, and some benign conditions may fulfill multiple criteria. The rule works best when applied by experienced clinicians who can integrate these findings with dermoscopic examination and patient history.
Meeting two or more ABCDEF criteria warrants dermatologic evaluation. Even a single criterion—particularly Hutchinson's sign or rapid change—justifies professional assessment. The consequences of delayed melanoma diagnosis far outweigh the minimal risks of unnecessary evaluation.
Understanding the distinct visual presentations helps with initial assessment, though professional evaluation remains essential for definitive diagnosis.
FeatureSubungual HematomaSubungual MelanomaPrimary colorsPurple, red, blue, dark brownBrown, black, dark brownColor uniformityGenerally uniform throughoutVariable shades within bandColor evolutionPurple → brown → yellow (fading)Stable or darkening brown-blackColor distributionDiffuse, irregular shapeLinear vertical band pattern
Hematoma patterns:
Melanoma patterns:
With hematoma:
With melanoma:
Dermatologists use dermoscopy (magnified visualization) to examine nail pigmentation more closely. This reveals patterns invisible to the naked eye:
Hematoma dermoscopy:
Melanoma dermoscopy:
The decision to seek medical evaluation depends on several factors, including trauma history, symptom progression, and presence of melanoma risk factors.
Seek prompt medical assessment (within days to weeks) if any of the following apply:
If the following conditions are met, monitoring for 2-3 months (fingernails) or 6-9 months (toenails) may be reasonable:
During watchful waiting:
If nail discoloration persists without change or improvement after two months in a fingernail or six months in a toenail, medical evaluation becomes necessary regardless of other factors. Normal bruise healing should show clear progress within these timeframes.
Certain groups should seek earlier evaluation:
While clinical examination provides strong clues, definitive diagnosis of subungual melanoma requires tissue sampling and pathological analysis.
The diagnostic process begins with:
History taking:
Visual inspection:
Dermoscopy:
A biopsy—tissue sampling for pathological examination—provides definitive diagnosis when:[1]
Nail matrix biopsy:
Excisional biopsy:
Nail plate avulsion with matrix biopsy:
The pathologist examines the tissue sample for:
Benign findings: Normal melanocyte distribution, no atypia, organized structure
Melanoma findings: Atypical melanocytes, irregular distribution, invasion into surrounding tissue, high mitotic rate
If melanoma is confirmed, additional testing determines the stage of disease:
Breslow thickness measurement: Depth of melanoma invasion (most important prognostic factor)
Sentinel lymph node biopsy: Checks if melanoma has spread to nearby lymph nodes
Imaging studies: CT, MRI, or PET scans to evaluate for distant metastasis in advanced cases
Blood tests: LDH levels may be elevated in metastatic disease
Survival rates depend heavily on the stage at diagnosis. Stage 1A subungual melanoma has approximately a 97% five-year survival rate, while Stage 4 has only 15-20% five-year survival, underscoring the critical importance of early detection.[2]

Treatment approaches for confirmed subungual melanoma depend on the stage at diagnosis, tumor thickness, and presence of metastasis.
Wide local excision:
Amputation:
Sentinel lymph node biopsy:
For advanced melanoma stages with metastasis:
Immunotherapy:
Targeted therapy:
Chemotherapy:
After treatment, regular monitoring includes:
Understanding common causes of subungual hematomas helps distinguish them from melanoma and guides prevention strategies.
Acute trauma:
Occupational hazards:
Footwear issues:
Medical conditions:
Proper footwear selection:
Nail care practices:
Activity modifications:
Medical management:
Frequent nail bruising without clear trauma may indicate:
Consult a healthcare provider if bruising occurs frequently without obvious cause.
Subungual melanoma represents a specific subtype of acral melanoma, which affects non-hair-bearing skin on palms, soles, and beneath nails.
Anatomical location:
Demographics:
Risk factors:
Subungual melanoma presents unique diagnostic difficulties:
Delayed recognition:
Mimicking conditions:
Biopsy reluctance:
Subungual melanoma generally has a worse prognosis than cutaneous melanoma at equivalent stages:
The critical factor: Early detection dramatically improves outcomes. Stage 1A subungual melanoma has approximately 97% five-year survival, emphasizing the importance of prompt evaluation of suspicious nail changes.[2]
While treatment principles remain similar to other melanomas, subungual melanoma presents unique considerations:
No, a nail bruise (subungual hematoma) cannot transform into melanoma. These are entirely different conditions with different cellular origins. A bruise results from blood vessel rupture and blood accumulation, while melanoma develops from malignant transformation of melanocytes. However, a melanoma can be mistaken for a bruise, leading to delayed diagnosis. Any "bruise" that doesn't heal within the expected 2-9 month timeframe should be evaluated for melanoma.
Subungual melanoma typically grows slowly over months to years, though growth rates vary considerably between individuals. The pigmented band may widen gradually, darken progressively, or remain relatively stable in appearance while the tumor invades deeper tissue. Some aggressive melanomas grow more rapidly, showing visible changes within weeks to months. Any observed change in size, color, or associated symptoms warrants prompt medical evaluation regardless of the rate of change.
Yes, though subungual melanoma in children is extremely rare. The vast majority of cases occur in adults aged 50-70 years.[2] When nail pigmentation appears in children, benign causes such as melanocytic activation, nevus, or trauma are far more likely. However, any persistent, changing, or concerning nail pigmentation in children should be evaluated by a pediatric dermatologist, particularly if there is a family history of melanoma or the child has a genetic syndrome predisposing to cancer.
No, while the classic presentation involves a brown-black vertical band (longitudinal melanonychia), subungual melanoma can present in other ways. Amelanotic melanoma (non-pigmented melanoma) can occur beneath the nail, appearing as a pink or flesh-colored nodule or area of nail dystrophy without dark pigmentation. Some melanomas present with nail plate destruction, bleeding, or ulceration without a visible pigmented band. Any unexplained persistent nail changes warrant evaluation.
While possible, subungual melanoma typically affects only one nail at a time.[2] Multiple nail involvement is much more commonly associated with benign conditions such as melanocytic activation from medications, systemic diseases, or normal ethnic variation in nail pigmentation. If multiple nails show similar pigmented bands, benign causes are more likely, though medical evaluation remains appropriate to confirm the diagnosis.
The vast majority of longitudinal melanonychia (dark lines under nails) are benign, particularly in individuals with darker skin tones where melanocytic activation is common. Estimates suggest that less than 1% of nail pigmentation cases represent melanoma in the general population. However, the percentage increases significantly in older adults (age 50+), those with single-digit involvement, bands wider than 3mm, irregular borders, or Hutchinson's sign. The exact percentage varies by population demographics and presence of risk factors.
A blood blister forms when blood collects between skin layers, creating a raised, fluid-filled bubble that typically appears suddenly after trauma. Subungual melanoma develops gradually as a flat pigmented band within the nail bed without fluid accumulation or raised appearance. Blood blisters resolve within days to weeks as the body reabsorbs the blood, while melanoma persists and may progress. Blood blisters are typically painful initially, whereas melanomas remain painless.
Unlike cutaneous melanoma, subungual melanoma has no clear association with UV radiation exposure, making traditional sun protection less relevant. No definitive prevention strategies exist for subungual melanoma. General melanoma risk reduction includes avoiding tanning beds, protecting skin from excessive sun exposure, and monitoring for changing moles or lesions. Individuals with family history of melanoma or personal history of previous melanoma should maintain heightened awareness and regular dermatologic surveillance.
Nail removal (avulsion) is not routinely necessary for melanoma evaluation. Dermoscopy (magnified examination) can often provide sufficient information to determine if biopsy is needed. When biopsy becomes necessary, the nail may be temporarily removed to access the nail matrix for tissue sampling, but this is done as part of the diagnostic procedure, not as a screening test. Unnecessary nail removal causes discomfort, temporary disability, and potential permanent nail dystrophy. Clinical evaluation and dermoscopy should guide the decision for biopsy.
First, consider whether you recall any recent trauma that might explain the discoloration. If trauma is likely and the appearance is consistent with a bruise (purple-red-blue coloring), photograph the nail and monitor for outward movement over 2-3 months (fingernails) or 6-9 months (toenails). If no trauma is recalled, the line is brown-black, you are over age 50, the band is wider than 3mm, or you notice Hutchinson's sign, schedule an evaluation with a dermatologist promptly. When in doubt, professional assessment provides peace of mind and ensures early detection if melanoma is present.
Most health insurance plans cover medically necessary procedures, including nail biopsy when melanoma is suspected based on clinical findings. Documentation of concerning features (ABCDEF criteria, dermoscopic findings, patient risk factors) supports medical necessity. Coverage varies by insurance plan and specific circumstances. Patients should verify coverage with their insurance provider before the procedure. The cost of biopsy is minimal compared to the potential cost of treating advanced melanoma that could result from delayed diagnosis. For more information about medical necessity and insurance coverage, see our cosmetic vs medical necessity insurance guide.
Current evidence does not establish a clear causal relationship between nail polish, gel manicures, or UV nail lamps and subungual melanoma development. The UV exposure from nail lamps is minimal compared to other UV sources and primarily affects the skin around the nail rather than the nail matrix where melanoma develops. However, nail polish and artificial nails can obscure nail changes, potentially delaying melanoma detection. Individuals at higher melanoma risk should consider periodic polish-free intervals to inspect nails or ensure their dermatologist examines nails during skin checks.
Distinguishing between a nail bruise and subungual melanoma requires careful attention to specific visual characteristics, growth patterns, and clinical features. While the vast majority of nail discoloration represents benign bruising or other non-cancerous conditions, the serious consequences of delayed melanoma diagnosis make appropriate evaluation essential.
The fundamental principle is simple: bruises heal and move, melanomas persist and may progress. A bruise under the nail will gradually shift toward the nail tip as the nail grows, typically resolving completely within 2-3 months for fingernails or up to 9 months for toenails. In contrast, a melanoma presents as a brown-black vertical band that remains in the same position on the nail bed, often widening or darkening over time.
If you notice dark discoloration under your nail:
Do not delay seeking medical assessment if you observe:
A dermatologist can perform dermoscopy, provide expert clinical assessment, and determine if biopsy is necessary. The minor inconvenience and cost of evaluation are negligible compared to the potential consequences of delayed melanoma diagnosis.
Subungual melanoma diagnosed at Stage 1A has approximately a 97% five-year survival rate, demonstrating that early detection leads to excellent outcomes.[2] However, delayed diagnosis allows progression to advanced stages with dramatically reduced survival rates. The average 2-3 year delay from symptom onset to diagnosis represents a critical window where intervention could save lives.
Maintain awareness of your nails during routine grooming. Remove nail polish periodically to inspect the nail bed. If you notice changes, document them and seek appropriate evaluation based on the features discussed in this guide. When in doubt, professional assessment provides definitive answers and peace of mind.
The distinction between a harmless bruise and a potentially life-threatening melanoma lies in careful observation, understanding of key differentiating features, and appropriate timing of medical evaluation. By applying the principles outlined in this melanoma on nails (subungual) vs bruise quick guide, you can make informed decisions about when to monitor and when to seek professional care.
For additional information about melanoma diagnosis and treatment, visit our comprehensive melanoma resource page or consult with a qualified dermatologist or melanoma specialist.
[1] Subungual Melanoma - https://www.moffitt.org/cancers/melanoma/diagnosis/types/subungual-melanoma/
[2] Is It A Bruise Or Maybe Subungual Melanoma - https://melanomacanada.ca/blog/is-it-a-bruise-or-maybe-subungual-melanoma/
[3] Toenail Hematoma Vs Melanoma Whats Under Your Nail - https://www.doctronic.ai/blog/toenail-hematoma-vs-melanoma-whats-under-your-nail/
[4] Subungual Melanoma - https://my.clevelandclinic.org/health/diseases/subungual-melanoma
[5] Subungual Hematoma - https://www.goodrx.com/conditions/musculoskeletal/subungual-hematoma
[6] Melanoma Affecting Toenails And Fingernails - https://www.mymelanomateam.com/resources/melanoma-affecting-toenails-and-fingernails
[7] Cutaneous Melanoma - https://melanoma.org/cutaneous-melanoma/
[8] Subungual Hematoma - https://www.healthline.com/health/subungual-hematomaSEO Meta Title and Description